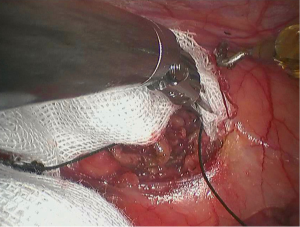
Robotic thoracic surgery of the anterior superior mediastinal bronchogenic cyst
Clinical data
Medical history
The patient, a 48-year-old man, was admitted due to “chest pain for 20 days” and “presence of anterior superior mediastinal mass”. He suffered from chest pain 20 days ago, which became severer when coughing. However, no tenderness or heart palpitations were noted. Chest CT at the local hospital showed a roundish hypodense lesion at the anterior superior mediastinum. Further abdominal ultrasound in a medical university-affiliated hospital showed no other abnormality. He then visited our hospital for further management. His general conditions were acceptable. The chest pain persisted, which became severer when coughing. He also had chest tightness and mildly irritating dry cough. However, he had no fever, night sweats, heart palpitations, or precordial discomfort. His mental status, physical performance, appetite, and sleep were normal, and the body weight did not obviously change. Urination and defecation were normal.
Physical examination
Physical examinations upon admission showed no obviously positive signs. The cervical and supraclavicular lymph nodes were not abnormally enlarged.
Auxiliary examination
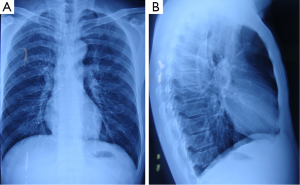
Chest X-ray had no abnormal findings in both lungs (Figure 1).
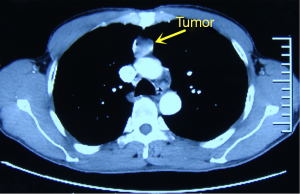
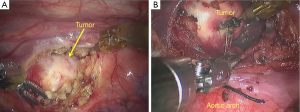
Chest CT: a roundish hypodense lesion sized 2.0 cm × 2.0 cm was visible in front of the ascending aorta in the anterior mediastinum. The lesion was somehow calcified, had smooth margin, and could be clearly distinguished from the surrounding tissues/vessels (Figure 2).
No obvious abnormality was found in abdominal/urinary ultrasound, ECG, echocardiography, pulmonary function test, blood gas analysis, and other biochemical tests.
Pre-operative preparation
Based on the imaging results, “a space-occupying lesion in the anterior mediastinum” was considered, and a benign lesion was highly possible. The patient had specific symptoms, and there were clear indications for a surgery, which was planned to be completed using da Vinci robotic system. Since the operations might be affected by the aortic arch and the lesion was located slightly near the right side, anterior mediastinal mass resection through the right chest would be performed.
Procedures
Anesthesia and body position
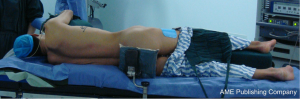
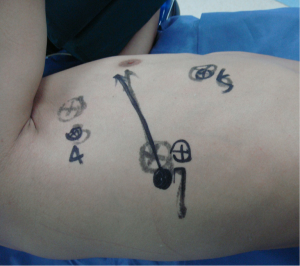
After the induction of general anesthesia, the patient was under double-lumen endotracheal intubation and directly underwent left-sided one-lung ventilation, so as to avoid the aggravation of pneumothorax caused by puncture. With his hands put in front of head, he was fixed in the left lateral decubitus position, with the head slightly tilted back (Figure 3).
Procedures
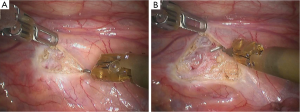
Incisions: a 1.2 cm camera port was created in the 6th intercostal space (ICS) right posterior axillary line, and two 0.8 cm working ports were separately made in the 4th ICS right posterior axillary line and the 5th ICS anterior axillary line (Figure 4).
During the thoracic cavity inspection, the camera was inserted via the camera port and found no obvious adhesion or effusion in the thoracic cavity.
The robot manipulators were connected from the left upper side over the patient’s head. A 12 mm trocar was placed at the camera port in the 6th ICS at posterior axillary line to be attached with the camera arm. The robot metal trocars were respectively attached to the bipolar coagulation forceps of the 2# arm (left hand) and the unipolar cautery hook of the 1# arm (right hand) at the incisions in the 4th ICS at posterior axillary line and 5th ICS at anterior axillary line.
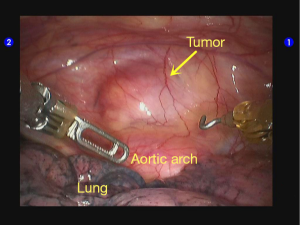
Inspection: the mass was located at the anterior superior mediastinum and below the mediastinal pleura. The mediastinal pleura were not involved. Tumor had smooth surface, without outward infiltration (Figure 5).
Surgical steps
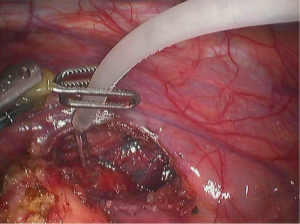
- Open the mediastinal pleura (Figure 6);
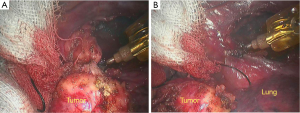
- Dissociate the tissues alongside the tumor capsule using the cautery hook (Figure 7);
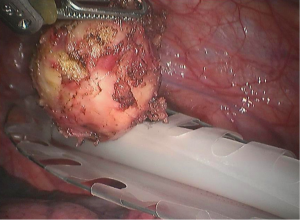
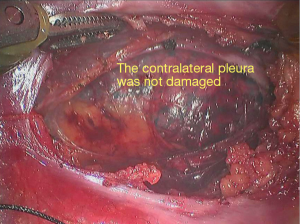
- The left side of the tumor is close to the mediastinal pleura and the left lung. The tumor was completely peeled off after careful separation (Figure 8);
- There was no bleeding or exudate on the wound surface (Figure 9);
- The dissolved hemostatic gauze glue was sprayed (Figure 10);
- After the right arm of the robot was withdrawn, the working port was enlarged to about 2.0 cm, via which the endoscopic retriever was inserted (Figure 11).
After the specimen was harvested, the tumor was complete, with intact capsule.
Frozen pathology suggested the possibility of teratoma, and the possibility of bronchogenic carcinoma needed to be ruled out.
Inspection showed that there was no obvious bleeding or exudate on the wound surface. The amounts of equipment, blood pads, and gauzes were correct.
The thoracic drainage tube was indwelled at the camera port and then well fixed. Close the chest after lung recruitment.
Note: if the visual field was affected by blood or exudate during the surgery, gauze can be used to clean it (Figure 12).
Postoperative treatment
The postoperative treatment was same as the conventional resection of mediastinal tumors. Symptomatic treatment was applied. The thoracic drainage tube was withdrawn 3 days after the surgery. Post-operative pathology: together with the immunohistochemical findings, a diagnosis of “bronchogenic cyst” was made.
Pathological diagnosis
Morphology
A roundish mass sized 2.5 cm × 2.0 cm × 2.0 cm was found at the right anterior mediastinum. It had capsule, with cystic sections. Bean dreg-like substances were found inside the cyst. The wall thickness was 0.2-0.4 cm. The mass was pale or grayish-yellow in color. It was moderately hard, although in some parts was hard.
Microscopy
Microscopy showed that the cyst wall contained fibrous tissue, which was lined with ciliated columnar epithelium, along with lymphocyte infiltration.
Immunohistochemistry
CK5/6 (+), CK8/18 (+), S-100 (-), SMA (+), CK7 (+), CK20 (+), CD34 (vascular +), CEA (+), Ki67 (+), and P53 (-).
Comment
The da Vinci system has been confirmed to a safe, accurate, and minimally invasive approach with promising clinical value. This technique is featured by small trauma, mild pain, quick recovery, and good cosmesis. Also, it can thoroughly remove the lesions with high safety and success rate. It has been gradually recognized and well accepted by patients. Now it has totally replaced the open surgeries or the conventional video-assisted thoracoscopic surgeries in treating the majority of anterior mediastinal lesions. As a promising technique, it will increasingly become a leading surgical approach along with the development of technology and know-hows over time.
Acknowledgements
Disclosure: The authors declare no conflict of interest.