Single-incision video-assisted thoracoscopic evaluation and emergent surgery for severe lung and chest wall injury after thoracic trauma in a water park
Introduction
Thoracic trauma is responsible for approximately 25% of trauma deaths (1). Although often managed with conservative treatment, in some cases emergent surgery is required for severe intrathoracic and chest wall lesions (tension pneumothorax, massive hemothorax, and lung or myocardial injuries) (2). We present a case of emergent surgery in a 23-year-old man with hemorrhagic shock due to massive lung and chest wall injury after thoracic trauma in a water slide.
Case presentation
A 23-year-old man suffered a high-energy impact in a water slide causing a severe thoracic left trauma. After initial first aid assessment the patient was transferred to the intensive care unit (ICU) of a local center. Auscultatory evaluation presented abolishment of respiratory murmur in the left hemithorax. A 24 Fr chest tube was inserted in left second intercostal space and with immediate output of 1 liter of blood and evidenced massive continuous air leak. In the next 10 minutes a total of 2 liters were drained and patient developed hemorrhagic shock and acute respiratory failure requiring endotracheal intubation, mechanical ventilation, blood replacement, and continuous perfusion of noradrenaline 1 mcg/kg/min to keep a normal blood pressure.
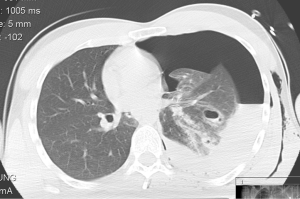
Subsequently, CT scan was performed showing left massive hemothorax, extensive parenchymal injuries in left lower lobe (LLL) and multiple rib fractures between ribs 9 to 12 (Figure 1). After initial stabilization the patient was sent to the reference hospital.
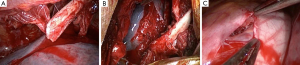
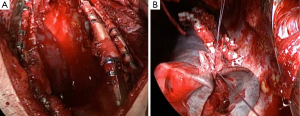
Upon arrival, fiberbronchoscopy in the ICU showed multiple haematic rests in left main bronchus without active bleeding but after aspiration we ruled out a tracheobronchial rupture. An urgent surgery was indicated so double-lumen endotracheal tube was placed and a 4-cm single incision VATS (SI-VATS) approach in the fifth intercostal space was performed. Several rib fractures with sharp surface had intracavity displacement and caused many lacerations in LLL (Figure 2A,B). One of those rib fragments injured the pericardium causing myocardical tear with no active bleeding and coronary preservation (Figure 2C). Due to the severe lesions in the chest wall with paradoxical motion, we indicated a 10-cm thoracotomy for chest wall repair just over the injured area. Rib fractures were stabilized with Judet plates (Figure 3A). After checking bronchial and vascular viability of LLL we proposed a lung parenchyma reconstruction with separate Vicryl sutures reinforced with teflon pledgets (pneumorraphy) in order to preserve the lung and avoid a lobectomy (Figure 3B).
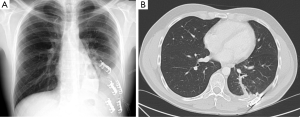
Blood loss during surgery was 1.5 liters. After placing two chest tubes and with a total operative time of 180 minutes, the patient was sent to a surgical critical care unit under mechanical ventilation. Noradrenaline requirements decreased gradually and weaning was performed 24 hours postoperatively. Chest tubes were removed on 3rd postoperative day without evidence of complications, and the patients was sent to the thoracic surgery ward. During the postoperative period, an isolated episode of acute hemoptysis was managed with conservative treatment, and there were no other complications. Postoperative electrocardiogram and echocardiography were normal. Patient was discharged on 14th postoperative day with normal chest X-ray (Figure 4A). CT scan 6 months after surgery shows postoperative normal changes (Figure 4B) and the patient has already recovered to his normal activity.
Discussion
Thoracic trauma is an important event with potential severe chest wall and intrathoracic organ injuries. In some series that involves patients with thoracic trauma, it constitutes approximately one third of all the trauma cases (3). Often, this condition can be managed with chest tube drainage and conservative support measures, which can be enough to stabilize the patient, remove the hemothorax and re-expand the lung (4). Nevertheless, emergent and urgent surgery should be considered when patient’s stability can not be achieved with previous measures. This case report describes a young man who suffered extreme thoracic trauma with hemodynamic instability due to chest wall and intrathoracic organ injuries. Lung parenchyma was massively affected with diffuse lacerations affecting to the LLL. Those injuries caused hemopneumothorax and subcutaneous emphysema. In cases like this, usually after place a chest tube is obtained a strong and continuous air leak which can mimic a tracheobronchial rupture that should be discarded with a bronchoscope evaluation within a surgical environment. We indicated a surgery with SI-VATS approach after secondary stabilization in order to define intrathoracic and chest wall injuries and once we check that chest wall was extensively affected we added a thoracotomy. Classically, it was considered hemodynamic instability as a total contraindication for VATS approach. Today, with the new advances in VATS and SI-VATS approach some authors report that hemodynamic instability should be considered as a relative contraindication due to advantages of thoracic inspection through VATS approach in a seriously damaged patient (5). Moreover, early VATS in thoracic trauma events can prevent serious complications such as empyemas or trapped lung (6).
In experienced hands, exploratory SI-VATS approach can assess injuries of diaphragm, chest wall, mediastinal areal, pericardium and lung parenchyma (5). Even if a thoracotomy becomes necessary, the initial thoracoscopy is useful to determine size, shape and extent of the incision, which also will minimize morbidity (7). If viable parenchyma can be preserved safely, lung preserving procedures such as lung pneumography should be considered, specially in young adults, after checking bronchial and vascular integrity.
Conclusions
In experienced teams of thoracic trauma SI-VATS can be the initial approach to explore, define and treat lesions secondary to thoracic trauma. If necessary, thoracotomy can be designed assisted through the minimally initial incision in order to do the less invasive approach and avoid unnecessary morbidity. Lung preserving techniques should be attempted first after vascular integrity assessment in order to avoid iatrogenic injury in a seriously damaged patient.
Acknowledgements
None.
Footnote
Conflicts of Interest: The authors have no conflicts of interest to declare.
Informed Consent: Written informed consent was obtained from the patient for publication of this manuscript and any accompanying images.
References
- Lin FC, Li RY, Tung YW, et al. Morbidity, mortality, associated injuries, and management of traumatic rib fractures. J Chin Med Assoc 2016;79:329-34. [Crossref] [PubMed]
- Gonçalves R, Saad R Jr. Thoracic damage control surgery. Rev Col Bras Cir 2016;43:374-81. [Crossref] [PubMed]
- Çakmak M, Nail Kandemir M. Study of 433 Operated Cases of Thoracic Trauma. Indian J Surg 2016;78:477-81. [Crossref] [PubMed]
- Molnar TF. Thoracic Trauma: Which Chest Tube When and Where? Thorac Surg Clin 2017;27:13-23. [Crossref] [PubMed]
- Fernández R, Delgado M, De la Torre M. Papel de la VATS en las urgencias torácicas. Manual de Urgencias en Cirugía Torácica. Madrid: Panamericana 2015:333-43.
- Billeter AT, Druen D, Franklin GA, et al. Video-assisted thoracoscopy as an important tool for trauma surgeons: a systematic review. Langenbecks Arch Surg 2013;398:515-23. [Crossref] [PubMed]
- Goodman M, Lewis J, Guitron J, et al. Video-assisted thoracoscopic surgery for acute thoracic trauma. J Emerg Trauma Shock 2013;6:106-9. [Crossref] [PubMed]