An update and review of cell-based wound dressings and their integration into clinical practice
Introduction
A chronic wound is defined as a wound that has failed to re-epithelialize after 3 months. Unfortunately, chronic wounds often fail to close due to an incomplete progression through one or more stages of wound healing including inflammation, proliferation, and remodeling (1,2). Over 4 million patients in the United States are affected with chronic wounds, and an excess of US $50 billion is spent every year on chronic wound treatments (3,4). Chronic wounds are often secondary to patient comorbidities, and can increase the cost of hospitalization and outpatient treatment. In our current era of increasing health care costs, an aging population, and increasing prevalence of obesity and diabetes, it is the important to identify novel therapeutic options for treating growing burden of chronic wounds (5).
Over 90% of all chronic wounds are a result of diabetic ulcers, venous stasis ulcers, and decubitus ulcers (6). Common features of chronic wounds include persistent infections, uncontrolled inflammation, formation of drug-resistant microbial biofilms, and loss of dermal and/or epidermal cells’ ability to respond to reparative stimuli (3). This failure to achieve adequate closure severely impacts patient quality of life due to significantly impaired mobility and chronic pain (5).
Current standard of care (SOC) for treating chronic wounds includes sharp surgical debridement, well-timed revascularization, infection control, off-loading or complete pressure relief for diabetic foot and pressure ulcers (PUs), and suitable compression for venous ulcers (2). Using SOC, closure rates for chronic wounds range from 21–35% and the recurrence rate is high, leaving much room for innovation (2).
Advances in cell biology and tissue engineering have led to an increase in the quantity and quality of biological wound dressings. Most cell-based dressings utilize a scaffold upon which cells are seeded. Scaffolds are designed to easily integrate with host tissue and provide an optimal environment for cell growth & differentiation. The cells themselves further encourage the progression of tissue formation (7). The sources of scaffold material and cells vary between products. Most studies examining cell-based dressings utilize a specific patient population presenting with wounds of at least 3 weeks duration and a co-morbidity, but few examine the potential for more broad utilization. Therefore, the aim of this study is to provide a comprehensive review of cell-based wound dressings currently available, and outline their potential integration into a clinical practice.
Methods
A literature search was performed using MEDLINE, Web of Knowledge, Cochrane Database of Systematic Reviews, and Google Scholar. Multiple search terms were used for this study including: “Grafix”, “EpiFix”, “AmnioExcel”, “NEOX”, “NEOX Wound Allograft”, “bilayer cellular matrix”, “human skin allograft”, “stem cell wound dressing”, “amniotic membrane dressing”, “Theraskin”, “Apligraf”, “Dermagraft”, “Graftskin”, “OrCel”, and “LeucoPatch”. These search results were then cross referenced with “biological dressing”, “cell-based wound dressing”, “wound healing”, “fibroblasts”, “platelet rich plasma”, “chronic wounds”, and “non-healing wounds”. Inclusion criteria were publication date between 1995 and 2016 and demonstration of utility in improving wound healing, especially the healing of chronic wounds. Exclusion criteria included non-English language articles, review articles, and meta-analysis due to small sample size. Items of interest included safety, time to complete wound healing or re-epithelialization, average wound size, patient co-morbidities such as venous stasis or diabetes mellitus, average dressing cost per square cm, source of tissue, scarring, and complication rate. A search of the above-listed databases yielded over 200 articles when trade name products, “biological dressing”, “cell-based wound dressing” were cross matched with “wound healing”, “chronic wounds”, and “non-healing wounds”. After review of all study titles, 83 abstracts were selected for analysis after elimination of articles that met exclusion criteria. A total of 76 abstracts were relevant to cell-based wound therapy, and these articles underwent final review in their entirety. Of these, 53 were included in this current review.
Amniotic & placental membranes
The original cell-based biologic dressing was fetal membrane, first introduced in 1910 for skin transplantation (8). Fetal membrane was subsequently found to be useful in the management of burns, creation of surgical dressings, and reconstruction of various tissues and organs (7). In these applications, amniotic membrane serves as an extracellular matrix (ECM), and delivers growth factors important for wound healing. These growth factors include transforming growth factor beta (TGF-β), epidermal growth factor (EGF), fibroblast growth factors (FGFs), and platelet-derived growth factors (PDGFs) (9). The amniotic membrane does not express HLA-A, B, or DR antigens and will not cause immunological rejection after transplantation (10).
Placental membrane also contains neonatal fibroblasts, mesenchymal stem cells (MSCs), and epithelial cells, which promote efficient wound healing (11). MSCs release soluble factors that stimulate proliferation and migration of the predominant cell types in the wound. MSCs also provide anti-scarring properties via paracrine release of vascular endothelial growth factor (VEGF) and hepatocyte growth factor (HGF) (12). Fibroblasts facilitate production of ECM along with growth factors, supplying the ideal environment for epidermis formation and wound closure (13).
Grafix (Osiris Therapeutics Inc., Columbia, MD, USA), a cryopreserved placental allograft, is indicated for acute & chronic wounds such as diabetic foot ulcers (DFUs), venous leg ulcers (VLUs), PUs, deep tunneling wounds, burns, pyoderma gangrenosum, epidermolysis bullosa, and surgical incisions & dehiscence. Grafix utilizes the native components of placental tissue, providing a three-dimensional ECM that contains various growth factors and living cells such as fibroblasts, epithelial cells, and MSCs. Studies have demonstrated that MSCs are a powerful stimulator of tissue repair and regeneration, playing a significant role in each of the three phases of wound healing (12,14,15).
Two clinical studies have examined the efficacy and safety of Grafix, and both studies showed that Grafix significantly increases wound closure rates. Lavery et al. (11) compared Grafix and SOC in treatment of DFUs, and found that 62% of Grafix patients achieved complete wound closure by week 12, compared to 21% of the SOC group (P=0.0001). Grafix patients exhibited a significantly shorter time to heal, significantly fewer adverse events (AEs), and significantly fewer wound-related infections compared with controls. Regulski et al. conducted a retrospective analysis on Grafix’s efficacy and safety in treatment of chronic wounds (16). In this study, 74.6% of total participants had failed to heal using other treatments, and 76.1% of these patients who received Grafix achieved complete wound closure by week 12. No AEs were attributed to Grafix and no wound recurrences were present after an average follow-up time of 20.4 months (Table 1).
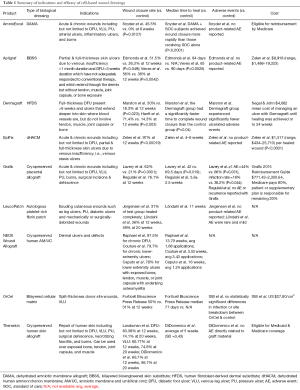
Full table
Dehydrated human amnion/chorion membrane (dHACM) allografts such as EpiFix (MiMedx Group Inc., Marietta, GA, USA) have shown promise in patients with neuropathic DFU and non-infected skin ulcers. EpiFix is made from human placentas, which are donated under informed consent and regulated by the Food and Drug Administration’s (FDA) Good Tissue Practice and American Association of Tissue Banks (AATB). Zelen et al. studied a cohort of 100 patients and assessed the efficacy of EpiFix and Apligraf (Organogenesis Inc., Canton, MA, USA) versus SOC over a duration of 12 weeks (17). Inclusion criteria were infection-free ulcers unresponsive to standard wound care for 4 weeks or longer, with adequate circulation to the affected extremity. Complete wound closure was achieved by 97% of EpiFix patients by week 12, compared to 73% of subjects treated with Apligraf, and 51% of subjects receiving SOC alone (adjusted P=0.00019) (Table 1). Additionally, patients in the EpiFix group used 94.4% less graft material and an average of 58% fewer grafts than Apligraf patients, resulting in an 83% lower median cost of graft material for the EpiFix group compared to the Apligraf group. Neither of these products contributed to any AEs reported.
AmnioExcel (Derma Sciences Inc., Princeton, NJ, USA) is a dehydrated amniotic membrane allograft (DAMA) used in the treatment of acute & chronic wounds such as DFUs, VLUs, PUs, arterial ulcers, inflammatory ulcers, and burns. DAMA base material is donated by appropriately screened mothers in accordance with AATB requirements, and DAMA is processed in compliance with the US FDA. Snyder et al. conducted a prospective, open-label, randomized trial examining the efficacy and safety of DAMA compared with SOC for closure DFUs (18). This study was conducted with 29 patients from eight clinical study sites, and revealed that 45.5% of patients in the DAMA + SOC group achieved complete wound closure by week 6, compared to 0% of SOC alone subjects (P=0.0083). DAMA + SOC patients achieved complete wound closure more rapidly than SOC alone patients (P<0.0001), and there appears to be no increased rate of AEs associated with use of DAMA (Table 1).
NEOX Wound Allograft (Amniox Medical, Atlanta, GA, USA) is a cryopreserved human amniotic membrane and umbilical cord (AM/UC) tissue dressing indicated for dermal ulcers and defects. Previous studies have examined umbilical cord’s ability to promote wound healing (19,20), and NEOX is unique in its combination of umbilical cord and amniotic tissues. In a retrospective chart review evaluating the efficacy of NEOX Wound Allograft in treatment of chronic DFU, 87.5% of wounds achieved complete epithelialization at an average healing time of 13.8 weeks (21).
A second retrospective review found that 79.7% of chronic foot and ankle wounds achieved complete epithelialization with NEOX at an average healing time of 5.53 weeks, using an average of 3.43 NEOX applications (19). A third retrospective study examined the efficacy and safety of NEOX cryopreserved umbilical cord in treatment of complex lower extremity ulcers involving exposed bone, muscle, tendon, or joint capsule within the background of underlying osteomyelitis (22). Seventy-eight percent of these complex wounds achieved complete closure, with a median time-to-heal of 16 weeks using an average of 1.24 applications of NEOX Wound Allograft (Table 1). These data suggest that cryopreserved umbilical cord is an effective treatment for complex leg ulcers with exposed subcutaneous structures, even in the presence of osteomyelitis.
Human skin allografts & bioengineered skin substitutes
Chronic wounds often lead to soft tissue defects that leave underlying structures such as muscle, bone, or tendon exposed increasing the risk of infection. These defects are usually addressed according to the reconstructive ladder, and skin grafts or vascularized tissue transfers are often needed in order to provide adequate coverage. Unfortunately, these surgical techniques require a donor site, increasing morbidity. Consequently, human skin allografts and bioengineered skin substitutes have been developed.
Theraskin (LifeNet Health, Virginia Beach, VA, USA) is a biologically active, cryopreserved human skin allograft indicated for repair of wounds such as DFU, VLU, PU, surgical dehiscence, necrotizing fasciitis, traumatic burns, and radiation burns. Tissue is harvested from screened cadaveric donors, and the allograft is processed in accordance with FDA and AATB regulations (23). Theraskin is unique in this category as it can be used over exposed bone, tendon, joint capsule, and muscle. A retrospective, single-center study by Landsman et al. examined patients with either a DFU or VLU whose average duration of wounds ranged from 17.9–20.6 weeks (23). For DFU treatment, 60.38% of wounds were closed by week 12 and 74.10% were closed at week 20. For VLU treatment, 60.77% of wounds were closed by week 12 and 74.60% were closed at week 20. The average number of Theraskin grafts utilized to achieve these closure rates was 2.03 by week 12 and 3.23 by week 20. Landsman et al. found that Theraskin did not contribute to any AEs (Table 1).
A prospective, randomized study by DiDomenico et al. compared the efficacy of Theraskin and Apligraf (Organogenesis, Canton, MA, USA), a bioengineered skin substitute, in treating DFUs (24). The authors hypothesized that Theraskin and Apligraf would yield the same results for wound closure rate and number of grafts required when treating DFU. DiDomenico et al. assessed 29 wounds from 28 patients—17 wounds received Apligraf and 12 wounds received Theraskin. At 12 weeks, Theraskin closed 66.7% of wounds and Apligraf closed 41.3% of wounds. At 20 weeks, the Theraskin closure rate remained at 66.7% and the Apligraf closure rate increased to 47.1%. Most patients received only a single application of either Theraskin or Apligraf, and the average wound closure time was 5 weeks for the Theraskin group and 6.86 weeks for the Apligraf group. No unexpected AE were reported in this study (Table 1).
Apligraf (Organogenesis Inc., Canton, MA, USA), is a bilayered bioengineered skin substitute (BBSS) containing a dermal layer of human fibroblasts in a bovine type I collagen lattice and an epidermal layer formed by human keratinocytes (25-28). Neonatal human foreskin is the source for the fibroblasts and keratinocytes, and Apligraf is FDA approved for treatment of partial & full-thickness skin ulcers due to venous insufficiency and DFU that have not appropriately responded to conventional therapy. Apligraf is indicated for wounds that extend through the dermis but do not involve muscle, tendon, joint capsule, or bone exposure. A prospective, randomized, multicenter, controlled study by Edmonds et al. compared the efficacy and safety of Apligraf compared to SOC in the treatment of neuropathic DFU (29). Seventy two patients with persistent full-thickness neuropathic ulcers were studied, and by week 12, 51.5% of Apligraf patients achieved complete wound closure compared to 26.3% of patients receiving standard care (P=0.049). The Apligraf group exhibited a median time to heal of 84 days, whereas no median time to heal could be determined for SOC patients because <50% of control subjects healed. Study treatments were not suspected to have contributed to any serious AEs. Veves et al. assessed 208 patients across 24 U.S. centers to evaluate the efficacy of Graftskin (former name of Apligraf) in treatment of chronic DFU (30). During the screening period, patients were treated with saline-moistened gauze, and patients who experienced a 30% or greater decrease in the size of their ulcer were excluded. At week 12, 56% of Graftskin patients achieved complete wound closure, compared with 38% of control patients (P=0.0042), with a median time to closure of 65 days for Graftskin patients and 90 days for control patients (P=0.0026) (Table 1). Patients received an average of 3.9 Graftskin applications over 12 weeks, and Graftskin caused no associated AEs.
Dermagraft (Smith and Nephew, Largo, FL, USA) is a cryopreserved human fibroblast-derived dermal substitute (HFDS) indicated for full-thickness DFU present for >6 weeks and ulcers that extend deeper into the skin but do not involve muscle, tendon, joint capsule or bone (31-34). The fibroblasts are derived from neonatal human foreskins and are cultured in vitro onto a bioabsorbable polyglactin mesh. As the fibroblasts proliferate across the mesh, “They secrete human dermal collagen, matrix proteins, growth factors, and cytokines to create a three-dimensional human dermal substitute containing metabolically active, living cells” (35). Fibroblasts from the dermis are relatively non-antigenic and do not express HLA-DR markers, therefore Dermagraft is not expected to cause an immune reaction (36,37).
Marston et al. assessed 314 patients across 35 U.S. centers to evaluate Dermagraft’s safety and efficacy in treatment of DFU. Eligible patients were diabetic adults with a foot ulcer between 1.0 and 20.0 cm2 that had been present for at least 2 weeks. The results showed that Dermagraft healed 30% of ulcers compared to 18% healed in the control group, and Dermagraft patients also had a significantly quicker time to complete wound closure than controls (P=0.04). Dermagraft patients were 1.7 times more likely to have complete wound closure than control patients, and the number of Dermagraft patients who developed ulcer-related AEs was significantly less than control. In addition, Hanft et al. assessed 46 patients to evaluate Dermagraft’s efficacy in treatment of chronic foot ulcers (38). All analyses were based on patients who experienced ulcers for a duration of 6 weeks or greater, and the Dermagraft group achieved significantly greater wound closure by week 12 compared to controls (71.4% vs. 14.3%, P=0.003). Dermagraft patients also experienced significantly faster time to complete wound closure compared to patients receiving control treatment (P=0.004). The number of patients who experienced AEs was comparable between treatment groups, and there were no adverse laboratory findings associated with the use of Dermagraft (Table 1).
OrCel (Ortec International Inc., New York, NY, USA) (39) is “A bilayered cellular matrix in which human allogeneic skin cells (epidermal keratinocytes & dermal fibroblasts) are cultured in two separate layers into a bovine type I collagen sponge. Dermal fibroblasts are cultured within the porous sponge side of the collagen matrix, while keratinocytes are cultured on the coated, non-porous side of the collagen matrix.” OrCel is FDA approved for non-infected split-thickness donor site wounds and is also pending FDA approval for treatment of VLUs. Still et al. enrolled 82 patients from 12 centers to evaluate OrCel’s efficacy compared with Biobrane-L® (synthetic wound dressing used as control) in treatment of split-thickness skin graft donor sites for management of burn injuries (40). Each patient had two equivalent donor sites, which were randomized to receive a single treatment of either OrCel or control. Patients included were age 1 year or older who sustained burns to 10–80% of their total body surface area, and had an anticipated life expectancy of 6 weeks or greater. OrCel treatment resulted in a significantly shorter time to wound closure, with OrCel treated sites healing a median of 7 days faster than control. No statistically significant difference was observed in site breakdown or infection between the OrCel and control. OrCel is estimated to cost about $1,000 per 36 cm2 (US $27.80/cm2). Data from recent clinical trials evaluating the efficacy of OrCel for treatment of VLU showed that 50% of OrCel patients achieved complete wound closure by week 12 compared with 31% of SOC subjects (Table 1). OrCel patients exhibited a median time to heal of 77 days, whereas no median time was determined for the control group. Results from the Diabetic Ulcer Pilot Study show that 47% of patients treated with OrCel achieved complete wound closure by week 12 compared to 23% of SOC treated patients.
Autologous platelet-rich plasma
In 1986 Knighton et al. published the first clinical demonstration that autologous platelet-derived wound healing factors can stimulate repair of chronic non-healing human wounds (41). Platelets release growth factors, cytokines, and interleukins that have crucial effects on healing mechanisms including angiogenesis, cell migration & proliferation, and synthesis of ECM proteins (42). Platelet rich plasma (PRP) refers to a 4- to 7-fold increase in the concentration of platelets in a small volume of plasma (at least 1,000,000 platelets/µL) and samples can be prepared from the patient’s own blood with relative ease(43,44). Due to its effectiveness in various aspects of tissue regeneration, PRP has been reported for a broad range of applications including general, orthopedic, cosmetic, dermatological, and oral & maxillofacial surgery (45-48).
LeucoPatch (Reapplix, Birkerød, Denmark) is a fibrin patch that contains concentrated leukocytes and platelets, which are quickly prepared from a small sample (18 mL) of donated blood (42,49-51). Blood is collected from the patient into a single-use LeucoPatch® Device, which in combination with the LeucoPatch 3CPTM Centrifuge, produces an autologous LeucoPatch® on demand. LeucoPatch is currently used in European healthcare centers to treat various non-healing wounds and is currently under evaluation for efficacy of DFU treatment in a randomized controlled clinical study expected to be complete in 2017. Reapplix recently received U.S. FDA 510(k) clearance for its 3C Patch SystemTM, which is indicated for the management of exuding cutaneous wounds such as PUs, leg ulcers, diabetic ulcers and mechanically or surgically-debrided wounds (49).
Jørgensen et al. evaluated the efficacy and safety of LeucoPatch in treating a variety of chronic wounds that did not appropriately respond to conventional treatments. Twelve patients with median wound duration of 34 months completed a full treatment course of LeucoPatch application once a week for 6 weeks, and 31% of wounds exhibited complete closure. LeucoPatch treatment reduced wound area by 64.7% at 6 weeks, and there was a significant increase in the proportion of granulation tissue within the wounds. The investigators did not consider any AEs to be related to the study treatment. Löndahl et al. examined non-ischemic Wagner grade 1 or 2 DFUs lasting a duration of 6 weeks or greater and a maximal area of 10 cm2 (52). LeucoPatch was applied once a week for up to 19 weeks or until the subject’s foot ulcer was completely epithelialized. Thirty-four percent of patients achieved complete epithelialization by week 12, and 52% achieved wound closure by week 20. Seventy-three percent of ulcers were healed within 20 weeks in patients who had ulcer durations less than 6 months. AE were mild and rare (Table 1).
Discussion
Decades of research into cell biology, growth factors, and ECM biology have led to an increased understanding of wound healing. Concomitant advances in the field of tissue engineering have led to new wound treatment options that offer significant advantages over the current SOC. While the mechanism of action for these products have yet to be fully elucidated, our review of cell-based biological dressings indicates that direct administration of cells to non-healing chronic wounds leads to significant improvement in various clinical scenarios. Possible benefits of cell based therapies include modulation of chronic inflammatory states, paracrine signaling that stimulates and attracts healthy cells to the wound bed, and transdifferentiation into effector cells that help to orchestrate wound closure.
Among dressings indicated for diabetic ulcers and ulcers due to venous insufficiency, EpiFix displayed the highest wound closure rate of 97% at 12 weeks (P=0.00019) in Zelen et al.’s study. While this data shows much promise, more studies are necessary to confirm the consistency of these results. However, with chronic non-healing wound treatment costs quoted as high as $30,000–40,000 per year (53), EpiFix is an example of a cost-effective alternative with a median price of $1,517 (range, $434–25,710) per healed wound (P<0.0001). While all the studies we reviewed indicated improved wound healing versus the SOC, there was minimal to no attention paid to the cost effectiveness of these cell-based therapies. At present, these newer treatments have high upfront costs. However, the next question that needs to be addressed is whether these higher upfront costs are associated with decreased overall cost to the health care system.
A reassuring finding from this review was that no significant AEs have been documented thus far with the use of cell-based matrices. While there is the potential for acute rejection reactions, allergic responses, infection, and other regional or systemic side effects, the overarching finding is that the approved cell based matrices can be used safely.
Overall the efficacy of cell-based wound dressings appears to cover a broad range of indications, and since most of these dressings have been available for 10 years or less, continued research is necessary to evaluate whether cell-based dressings could potentially replace the current SOC altogether. Nevertheless, it is encouraging to have new modalities to treat challenging chronic wounds, and likely that further optimization will be associated with improved outcomes.
Acknowledgements
None.
Footnote
Conflicts of Interest: The authors have no conflicts of interest to declare.
References
- Werdin F, Tennenhaus M, Schaller HE, et al. Evidence-based management strategies for treatment of chronic wounds. Eplasty 2009;9:e19. [PubMed]
- Gibbons GW. Grafix®, a Cryopreserved Placental Membrane, for the Treatment of Chronic/Stalled Wounds. Adv Wound Care (New Rochelle) 2015;4:534-44. [Crossref] [PubMed]
- Frykberg RG, Banks J. Challenges in the Treatment of Chronic Wounds. Adv Wound Care (New Rochelle) 2015;4:560-82. [Crossref] [PubMed]
- Fife CE, Carter MJ. Wound Care Outcomes and Associated Cost Among Patients Treated in US Outpatient Wound Centers: Data From the US Wound Registry. Wounds 2012;24:10-7. [PubMed]
- Sen CK, Gordillo GM, Roy S, et al. Human skin wounds: a major and snowballing threat to public health and the economy. Wound Repair Regen 2009;17:763-71. [Crossref] [PubMed]
- Mustoe TA, O'Shaughnessy K, Kloeters O. Chronic wound pathogenesis and current treatment strategies: a unifying hypothesis. Plast Reconstr Surg 2006;117:35S-41S. [Crossref] [PubMed]
- Niknejad H, Peirovi H, Jorjani M, et al. Properties of the amniotic membrane for potential use in tissue engineering. Eur Cell Mater 2008;15:88-99. [Crossref] [PubMed]
- Davis JW. Skin transplantation with a review of 550 cases at the Johns Hopkins Hospital. Johns Hopkins Med J 1910;15:307.
- Serena TE, Carter MJ, Le LT, et al. A multicenter, randomized, controlled clinical trial evaluating the use of dehydrated human amnion/chorion membrane allografts and multilayer compression therapy vs. multilayer compression therapy alone in the treatment of venous leg ulcers. Wound Repair Regen 2014;22:688-93. [Crossref] [PubMed]
- Dua HS, Azuara-Blanco A. Amniotic membrane transplantation. Br J Ophthalmol 1999;83:748-52. [Crossref] [PubMed]
- Lavery LA, Fulmer J, Shebetka KA, et al. The efficacy and safety of Grafix(®) for the treatment of chronic diabetic foot ulcers: results of a multi-centre, controlled, randomised, blinded, clinical trial. Int Wound J 2014;11:554-60. [Crossref] [PubMed]
- Maxson S, Lopez EA, Yoo D, et al. Concise review: role of mesenchymal stem cells in wound repair. Stem Cells Transl Med 2012;1:142-9. [Crossref] [PubMed]
- Wong T, McGrath JA, Navsaria H. The role of fibroblasts in tissue engineering and regeneration. Br J Dermatol 2007;156:1149-55. [Crossref] [PubMed]
- Shin L, Peterson DA. Human mesenchymal stem cell grafts enhance normal and impaired wound healing by recruiting existing endogenous tissue stem/progenitor cells. Stem Cells Transl Med 2013;2:33-42. [Crossref] [PubMed]
- Ennis WJ, Sui A, Bartholomew A. Stem Cells and Healing: Impact on Inflammation. Adv Wound Care (New Rochelle) 2013;2:369-78. [Crossref] [PubMed]
- Regulski M, Jacobstein DA, Petranto RD, et al. A retrospective analysis of a human cellular repair matrix for the treatment of chronic wounds. Ostomy Wound Manage 2013;59:38-43. [PubMed]
- Zelen CM, Serena TE, Gould L, et al. Treatment of chronic diabetic lower extremity ulcers with advanced therapies: a prospective, randomised, controlled, multi-centre comparative study examining clinical efficacy and cost. Int Wound J 2016;13:272-82. [Crossref] [PubMed]
- Snyder RJ, Shimozaki K, Tallis A, et al. A Prospective, Randomized, Multicenter, Controlled Evaluation of the Use of Dehydrated Amniotic Membrane Allograft Compared to Standard of Care for the Closure of Chronic Diabetic Foot Ulcer. Wounds 2016;28:70-7. [PubMed]
- Couture M. A. Single-center, Retrospective Study of Cryopreserved Umbilical Cord for Wound Healing in Patients Suffering From Chronic Wounds of the Foot and Ankle. Wounds 2016;28:217-25. [PubMed]
- Harris DT, Rogers I. Umbilical cord blood: a unique source of pluripotent stem cells for regenerative medicine. Curr Stem Cell Res Ther 2007;2:301-9. [Crossref] [PubMed]
- Raphael A. A single-centre, retrospective study of cryopreserved umbilical cord/amniotic membrane tissue for the treatment of diabetic foot ulcers. J Wound Care 2016;25 Suppl 7:S10-7. [Crossref] [PubMed]
- Caputo WJ, Vaquero C, Monterosa A, et al. A retrospective study of cryopreserved umbilical cord as an adjunctive therapy to promote the healing of chronic, complex foot ulcers with underlying osteomyelitis. Wound Repair Regen 2016;24:885-93. [Crossref] [PubMed]
- Landsman AS, Cook J, Cook E, et al. A retrospective clinical study of 188 consecutive patients to examine the effectiveness of a biologically active cryopreserved human skin allograft (TheraSkin®) on the treatment of diabetic foot ulcers and venous leg ulcers. Foot Ankle Spec 2011;4:29-41. [Crossref] [PubMed]
- DiDomenico L, Landsman AR, Emch KJ, et al. A prospective comparison of diabetic foot ulcers treated with either a cryopreserved skin allograft or a bioengineered skin substitute. Wounds 2011;23:184-9. [PubMed]
- Zaulyanov L, Kirsner RS. A review of a bi-layered living cell treatment (Apligraf) in the treatment of venous leg ulcers and diabetic foot ulcers. Clin Interv Aging 2007;2:93-8. [Crossref] [PubMed]
- Curran MP, Plosker GL. Bilayered bioengineered skin substitute (Apligraf): a review of its use in the treatment of venous leg ulcers and diabetic foot ulcers. BioDrugs 2002;16:439-55. [Crossref] [PubMed]
- Fivenson D, Scherschun L. Clinical and economic impact of Apligraf for the treatment of nonhealing venous leg ulcers. Int J Dermatol 2003;42:960-5. [Crossref] [PubMed]
- Langer A, Rogowski W. Systematic review of economic evaluations of human cell-derived wound care products for the treatment of venous leg and diabetic foot ulcers. BMC Health Serv Res 2009;9:115. [Crossref] [PubMed]
- Edmonds M, European and Australian Apligraf Diabetic Foot Ulcer Study Group. Apligraf in the treatment of neuropathic diabetic foot ulcers. Int J Low Extrem Wounds 2009;8:11-8. [Crossref] [PubMed]
- Veves A, Falanga V, Armstrong DG, et al. Graftskin, a human skin equivalent, is effective in the management of noninfected neuropathic diabetic foot ulcers: a prospective randomized multicenter clinical trial. Diabetes Care 2001;24:290-5. [Crossref] [PubMed]
- Harding K, Sumner M, Cardinal M. A prospective, multicentre, randomised controlled study of human fibroblast-derived dermal substitute (Dermagraft) in patients with venous leg ulcers. Int Wound J 2013;10:132-7. [Crossref] [PubMed]
- Hart CE, Loewen-Rodriguez A, Lessem J. Dermagraft: Use in the Treatment of Chronic Wounds. Adv Wound Care (New Rochelle) 2012;1:138-41. [Crossref] [PubMed]
- Omar AA, Mavor AI, Jones AM, et al. Treatment of venous leg ulcers with Dermagraft. Eur J Vasc Endovasc Surg 2004;27:666-72. [Crossref] [PubMed]
- Segal L, John S. The Use of Dermagraft in Neuropathic Foot Ulcers in People with Diabetes: An Economic Analysis for Australia. Primary Intention: The Australian Journal of Wound Management 2002;10:49-50, 52-54, 56-57.
- Naughton G, Mansbridge J, Gentzkow G. A metabolically active human dermal replacement for the treatment of diabetic foot ulcers. Artif Organs 1997;21:1203-10. [Crossref] [PubMed]
- Kern A, Liu K, Mansbridge J. Modification of fibroblast gamma-interferon responses by extracellular matrix. J Invest Dermatol 2001;117:112-8. [Crossref] [PubMed]
- Marston WA, Hanft J, Norwood P, et al. The efficacy and safety of Dermagraft in improving the healing of chronic diabetic foot ulcers: results of a prospective randomized trial. Diabetes Care 2003;26:1701-5. [Crossref] [PubMed]
- Hanft JR, Surprenant MS. Healing of chronic foot ulcers in diabetic patients treated with a human fibroblast-derived dermis. J Foot Ankle Surg 2002;41:291-9. [Crossref] [PubMed]
- Martin LK, Kirsner RS. Use of a meshed bilayered cellular matrix to treat a venous ulcer. Adv Skin Wound Care 2002;15:260-262, 264. [Crossref] [PubMed]
- Still J, Glat P, Silverstein P, et al. The use of a collagen sponge/living cell composite material to treat donor sites in burn patients. Burns 2003;29:837-41. [Crossref] [PubMed]
- Knighton DR, Ciresi KF, Fiegel VD, et al. Classification and treatment of chronic nonhealing wounds. Successful treatment with autologous platelet-derived wound healing factors (PDWHF). Ann Surg 1986;204:322-30. [Crossref] [PubMed]
- Perez-Zabala E, Basterretxea A, Larrazabal A, et al. Biological approach for the management of non-healing diabetic foot ulcers. J Tissue Viability 2016;25:157-63. [Crossref] [PubMed]
- Jee CH, Eom NY, Jang HM, et al. Effect of autologous platelet-rich plasma application on cutaneous wound healing in dogs. J Vet Sci 2016;17:79-87. [Crossref] [PubMed]
- Marx RE. Platelet-rich plasma (PRP): what is PRP and what is not PRP? Implant Dent 2001;10:225-8. [Crossref] [PubMed]
- Foster TE, Puskas BL, Mandelbaum BR, et al. Platelet-rich plasma: from basic science to clinical applications. Am J Sports Med 2009;37:2259-72. [Crossref] [PubMed]
- Leo MS, Kumar AS, Kirit R, et al. Systematic review of the use of platelet-rich plasma in aesthetic dermatology. J Cosmet Dermatol 2015;14:315-23. [Crossref] [PubMed]
- Marx RE, Carlson ER, Eichstaedt RM, et al. Platelet-rich plasma: Growth factor enhancement for bone grafts. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 1998;85:638-46. [Crossref] [PubMed]
- Rozman P, Bolta Z. Use of platelet growth factors in treating wounds and soft-tissue injuries. Acta Dermatovenerol Alp Pannonica Adriat 2007;16:156-65. [PubMed]
- Jørgensen B, Karlsmark T, Vogensen H, et al. A pilot study to evaluate the safety and clinical performance of Leucopatch, an autologous, additive-free, platelet-rich fibrin for the treatment of recalcitrant chronic wounds. Int J Low Extrem Wounds 2011;10:218-23. [Crossref] [PubMed]
- Driver VR, Hanft J, Fylling CP, et al. A prospective, randomized, controlled trial of autologous platelet-rich plasma gel for the treatment of diabetic foot ulcers. Ostomy Wound Manage 2006;52:68-70, 72, 74 passim. [PubMed]
- Esat Duymus M, Temel S, Ozer H, et al. Comparison of the Effects of Plateletrich Plasma Prepared in Various Forms on the Healing of Dermal Wounds in Rats. Wounds 2016;28:99-108. [PubMed]
- Löndahl M, Tarnow L, Karlsmark T, et al. Use of an autologous leucocyte and platelet-rich fibrin patch on hard-to-heal DFUs: a pilot study. J Wound Care 2015;24:172-4, 176-8. [Crossref] [PubMed]
- Fetterolf DE, Snyder RJ. Scientific and clinical support for the use of dehydrated amniotic membrane in wound management. Wounds 2012;24:299-307. [PubMed]


