
Re-appearance of the SARS-CoV-2 virus nucleic acid in patients recovering from COVID-19
As of March 13, 2020, the ongoing pandemic of COVID-19 worldwide has caused more than 130,000 infections and the death toll near 5,000. A study of 72,314 Chinese patient records revealed that most cases (80.9%) had mild symptoms while the elderly and people with comorbid conditions such as hypertension and diabetes are at higher risk of severe disease (1). So far, more than 60,000 patients have recovered from COVID-19 pneumoniae and are discharged home based on the Novel Coronavirus Infection Diagnosis and Treatment Plan released by the China National Health Commission (CNHC). The discharge standards include: (I) body temperature back to normal for more than 3 days; (II) respiratory symptoms significantly improved; (III) chest CT images of bilateral lungs showing significant absorption of acute exudative lesions; and (IV) negative nucleic acid test for two consecutive respiratory specimens with at least 1-day sampling interval.
After hospital discharge, recovered patients are advised to stay isolated at home for another 14 days because of their lower immune functions. Re-examination of the recovered patients is recommended after 2 weeks of discharge. Recently, four patients recovered from COVID-19 were tested positive again via RT-PCR in the affiliated Zhongnan Hospital of Wuhan University (2), which indicates that recovered patients might still carry the SARS-CoV-2 virus. Considering the large number of infected patients and the high recovery rate in China, it is possible that there might be many recovered or recovering patients still carrying the virus. However, whether recovered patients are contagious or not is still not clear and requires further investigation. In general, these recovered SARS-CoV-2 carriers make the control and prevention of COVID-19 infection more challenging and complicated (3).
In this correspondence, we reported a family cluster of four patients who were discharged from hospital and were recovering from COVID-19 in Xuzhou, China. All cases stayed isolated in independent rooms in a hotel after discharge, among which two cases (father and daughter 2) turned into SARS-CoV-2 positive during virus re-examination through nuclei acid test (Shanghai BioGerm Medical Biotechnology Co., Ltd., Shanghai, China). The father is a 56-year-old farmer (Case 1) with Wuhan travel history. He arrived in Xuzhou on Jan 14, 2020 and was the first imported COVID-19 case in the city. Between January 14 and January 22, he had close contacts with his two daughters, a 32-year-old pregnant teacher (Case 2) and a 21-year-old undergraduate student (Case 3). Since January 15, the man took care of his 42-year-old son-in-law (Case 4, husband of Case 2) admitted to the affiliated hospital of Xuzhou Medical University until January 20. Epidemiological study revealed that Case 1 was the index patient, leading to the infection of other 3 family members. On Jan 29, Case 1 was in severe conditions (breaths per minute ≥30 and oximetry saturation ≤93%). After medical treatment, he was discharged on Feb 9. On Feb 26 and 27, two consecutive nucleic acid tests showed positive results for SARS-CoV-2 through throat swab samples. Another throat swab test for SARS-CoV-2 on Feb 29 was still positive. On March 1 and 2, nuclei acid tests on throat swab samples and anal samples turned into negative. Case 3 is the younger daughter of Case 1. She was also discharged on Feb 9 and re-examed on Feb 26 and 27. Nucleic acid tests were consistently negative on samples from throat swab. However, tests on anal swab samples on Feb 26 and Feb 28 were positive. Nucleic acid tests on anal swab samples turned into negative on March 2. For the two cases, although being re-tested positive for SARS-CoV-2 infection after discharge, whether virus viability nor the quantitative virus load was not available. As for clinical diagnosis, chest CT scanning images for the two patients with SARS-CoV-2 nuclei acid re-appearance showed obvious absorption of bilateral lung lesions when compared with that at discharge, though high-density areas still exist, which indicates continuing recovery. The other two cases (Case 2 and Case 4) kept negative for SARS-CoV-2 tests after discharge. For a timeline of the progression in the clinical course in the family cluster, please refer to Figure 1.
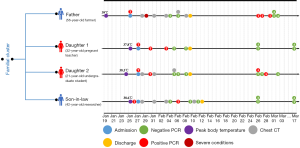
Discovery of SARS-CoV-2 nucleic acid reappearance in recovering patients is alarming. It raises the question of could the low accuracy of nucleic acid tests be responsible for the false negative result during hospitalization or the false positive result during re-examination (4)? In addition, since other swab tests (samples of urea, anus, and blood) are not included in the latest national standard diagnosis plan in China, should it be more reliable to test multiple samples than just throat swab test? What is also interesting to investigate is the viability of viruses detected in samples. Most importantly, are the SARS-CoV-2 carriers at recovering stage still contagious? Answers to these questions are urgently needed and could provide better guidelines for COVID-19 prevention and control. In sum, SARS-CoV-2 only recently jumped from bats to human beings through unknown intermediate hosts (5), there are still many things that we currently do not know about it. More epidemiological, clinical, and molecular studies are needed to get an overall understanding of the cunning virus.
Acknowledgments
We express our special appreciation and thanks to Professor Minglong Chen, Professor Peisheng Jin, and Professor Xianliang Yan for their advices and guidance on this study.
Funding: None.
Footnote
Conflicts of Interest: All authors have completed the ICMJE uniform disclosure form (available at http://dx.doi.org/10.21037/atm-20-2491). BG reports serving an unpaid editorial board member (managing editor) of Annals of Translational Medicine at current stage. The other authors have no other conflicts of interest to declare.
Ethical Statement: The authors are accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved. This study was approved by the Ethics Committee of Xuzhou Medical University (No. XYFY2020-KL016-01). Patient consents were obtained for publication.
Open Access Statement: This is an Open Access article distributed in accordance with the Creative Commons Attribution-NonCommercial-NoDerivs 4.0 International License (CC BY-NC-ND 4.0), which permits the non-commercial replication and distribution of the article with the strict proviso that no changes or edits are made and the original work is properly cited (including links to both the formal publication through the relevant DOI and the license). See: https://creativecommons.org/licenses/by-nc-nd/4.0/.
References
- Novel Coronavirus Pneumonia Emergency Response Epidemiology Team. The epidemiological characteristics of an outbreak of 2019 novel coronavirus diseases (COVID-19) in China. Zhonghua Liu Xing Bing Xue Za Zhi 2020;41:145-51. [PubMed]
- Lan L, Xu D, Ye G, et al. Positive RT-PCR test results in patients recovered from COVID-19. JAMA 2020;323:1502-3. [Crossref] [PubMed]
- Bai Y, Yao L, Wei T, et al. Presumed asymptomatic carrier transmission of COVID-19. JAMA 2020;323:1406-7. [Crossref] [PubMed]
- Ai T, Yang Z, Hou H, et al. Correlation of chest CT and RT-PCR testing in coronavirus disease 2019 (COVID-19) in China: a report of 1014 cases. Radiology 2020.200642. [Epub ahead of print]. [Crossref] [PubMed]
- Zhou P, Yang XL, Wang XG, et al. A pneumonia outbreak associated with a new coronavirus of probable bat origin. Nature 2020;579:270-3. [Crossref] [PubMed]


