
Polymorphisms in microRNA let-7 binding sites of the HIF1AN and CLDN12 genes can predict pathologic complete response to taxane- and platinum-based neoadjuvant chemotherapy in breast cancer
Introduction
MicroRNAs (miRNAs) are small, single-stranded molecules approximately 21 nucleotides in length (1). They are involved in the development and progression of malignant tumours, mainly through the post-transcriptional modulation of various physiological and pathological pathways (2-4). Several studies reported that miRNA may influence patient response to chemotherapy. The miRNA let-7 family and its role in oncogene regulation has also been studied. The let-7 family of miRNAs is involved in the suppression of several oncogenes (5-7), and let-7 is therefore considered a tumour suppressor miRNA. One study found that lower expression of let-7a miRNA might induce chemoresistance in breast cancer (BC) by enhancing cellular apoptosis (8), whereas other studies showed that let-7 expression is associated with response to chemotherapeutics (9-12).
Neoadjuvant chemotherapy is increasingly used in women with newly diagnosed early BC especially locally advanced breast cancer (LABC) (13,14). The advantage of neoadjuvant chemotherapy is that breast-conserving surgery can be performed more frequently (15). In addition, it offers the opportunity to directly assess a tumour’s response to therapy. Pathological complete response (pCR) is defined as the absence of invasive cancer, and it has been demonstrated that pCR after neoadjuvant chemotherapy is associated with better long-term survival (16-18). Among the women who receive neoadjuvant chemotherapy, the clinical response rate is as high as 70%, but only approximately 15–30% of patients achieve pCR (13,14,19). Novel predictive biomarkers that can predict tumour response prior to chemotherapy are valuable for individualized treatment decisions and to maximize efficacy in cancer patients.
MiRNAs regulate gene expression by base pairing with sequences within the 3’-untranslated region (UTR), 5’-UTR, and coding sequence regions of target mRNAs (20). Several recent studies have emphasized that polymorphisms in miRNA binding sites are predictors of response to chemotherapy in patients with malignant tumours (21-24). Moreover, it has also been reported that miRNA let-7 regulates the HIF1AN (25,26) and CLDN12 genes (27). Hypoxia-inducible factor 1-alpha inhibitor is a protein that is encoded by the HIF1AN gene. HIF1AN expression and differential cellular localization have been shown to be associated with shorter survival in BC (28). Claudins, which are the most important tight junction proteins, are also linked with cancer progression and metastasis. Claudin-12 belongs to a group of claudins and is encoded by CLDN12 gene. In our previous study, we found that polymorphisms located in the HIF1AN and CLDN12 genes were associated with BC susceptibility. Whether the polymorphisms located in the HIF1AN and CLDN12 genes have a predictive role in response to neoadjuvant chemotherapy in LABC warrants further investigation.
In this study, we selected two let-7 miRNA-related single nucleotide polymorphisms (mirSNPs) (rs11292 located in the HIF1AN gene and rs1017105 located in the CLDN12 gene). We hypothesized that genetic variations in miRNA let-7 binding sites located in the HIF1AN and CLDN12 genes could predict response to taxane- and platinum-based neoadjuvant chemotherapy in BC. In this study, we identified the rs11292 and rs1017105 SNPs in participants from two prospective, phase II studies (29), in which patients received weekly paclitaxel and cisplatin as neoadjuvant chemotherapy.
Methods
Study population
From October 2013 until November 2016, 130 patients with LABC were recruited for this study. The inclusion criteria were females aged between 18 and 70 years with histologically confirmed and untreated large operable BC (T size ≥2 cm and N0–2). Patients with other malignancies were excluded. Other inclusion and exclusion criteria are described elsewhere (29). Patients enrolled in this study were participants from two open-label, prospective, phase II trials. In these two trials, patients were scheduled to receive an intravenous (i.v.) infusion of 80 mg/m2 paclitaxel weekly on day 1 for 16 weeks and 25 mg/m2 cisplatin on days 1, 8, and 15 every 28 days. Patients with human epidermal growth factor receptor 2 (HER2)-positive cancer could use concomitant trastuzumab on a weekly basis. Written informed consent was obtained from each subject. For each subject, a 5 mL peripheral blood sample was collected and stored at −80 °C. The DNA was extracted from the peripheral blood samples of all subjects using a Qiagen DNA blood kit (Qiagen NV, Venlo, The Netherlands) according to the manufacturer’s protocols. The study was approved by the ethics committee of Renji Hospital, Shanghai Jiao Tong University. This study was conducted in accordance with the Declaration of Helsinki. Detailed characteristics of the patients enrolled in this study are shown in Table S1.
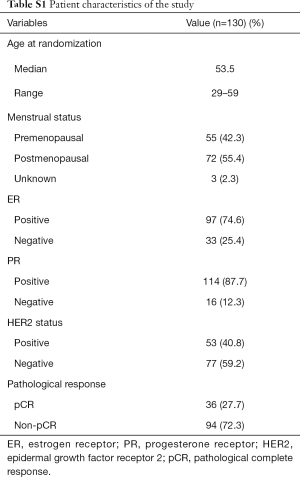
Full table
Histopathologic response
The pCR was evaluated in the surgical specimens’ post-chemotherapy and was defined as the absence of invasive cancer in the breast, with or without residual non-invasive intraductal carcinoma. All cases with residual invasive cancer of any size were classified as non-pCR.
Selection of SNPs in the HIF1AN and CLDN12 genes
First, we searched the miRBase (www.mirbase.org, Release 22), TargetScan (http://www.targetscan.org/, Release 7.2) and UCSC Genome Browser (http://genome.cse.ucsc.edu) databases to identify potential target genes of miRNA let-7. Second, we selected potential target genes of miRNA let-7 that are associated with malignant characteristics of BC, such as proliferation, angiogenesis, invasion, metastasis or inhibition of apoptosis. We screened the SNP loci that cover the extension of 2 kb at both sides of the let-7-binding sites in the target genes. We then screened for SNP loci in the binding sites of miRNA let-7 with low-binding free energy. Table 1 lists the characteristics of the candidate loci.

Full table
SNP genotyping
SNP genotyping was performed at Shanghai Bene-gene Biotechnology Co., Ltd. (Shanghai, People’s Republic of China) with the MassARRAY system (Sequenom, San Diego CA, USA) using matrix-assisted laser desorption ionization-time of flight (MALDI-TOF) mass spectrometry. Detailed information on the primers is shown in Table 2.

Full table
Statistical analysis
Genotype distributions were tested for adherence to the Hardy-Weinberg equilibrium (HWE). Associations among tumour-relevant biomarkers, genotype and pCR were evaluated using Student’s t-test for continuous variables and chi-square or Fisher’s exact tests for non-categorical variables. The modified odds ratios (ORs) with their 95% confidence intervals (CIs) were calculated by univariate and multivariate logistic regression analyses to explore the association of genotype with pCR. All statistical analyses were calculated by Stata 14.0 (StataCorp LP, College Station, TX, USA).
Results
Association of SNPs in the HIF1AN and CLDN12 genes with the histopathological characteristics of BC patients
Between 2013 and 2016, 130 patients with LABC were recruited for this study. The genotypic distribution, which was tested for deviation from HWE, showed no deviation for HIF1AN rs11292 or CLDN12 rs1017105 (data not shown). The association of the rs11292 and rs1017105 genotypes with the clinicopathologic parameters of primary BC was noted. No significant correlation was observed between these two genotypes and clinicopathologic features, including age, menstrual status, or estrogen receptor (ER), progesterone receptor (PR) and HER2 status.
Relationship of the SNPs in the HIF1AN and CLDN12 genes with response to neoadjuvant chemotherapy
Thirty-six of 130 (27.7%) patients achieved pCR after neoadjuvant chemotherapy. The pCR rate was 27.6% in patients with the HIF1AN rs11292 TT genotype and 43.5% in patients with the TC genotype. In the univariate analysis, no significant differences were detected in the rs11292 genotype between the pCR and non-pCR patients. In the multivariate analysis, significant differences were detected in the codominant, dominant and overdominant models of rs11292 between these two groups (P<0.05), which suggests that the rs11292 genotype is associated with response to neoadjuvant chemotherapy. The genotype distributions in the pCR and non-pCR patients are shown in Table 3. In the codominant model, women carrying the TC (OR =4.46, 95% CI: 1.26–15.78, P=0.02) genotype of HIF1AN rs11292 had a higher pCR rate than those carrying the TT genotype. In the dominant model, women carrying the TC + CC (OR =3.41, 95% CI: 1.02–11.33, P=0.046) genotypes of HIF1AN rs11292 had a higher pCR rate than those carrying the TT genotype. In the overdominant model, women carrying the TC (OR =4.63, 95% CI: 1.31–16.33, P=0.017) genotype of HIF1AN rs11292 had a higher pCR rate than those carrying the TT + CC genotypes (Table 3).
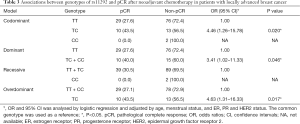
Full table
The pCR rate was 18.8% in patients with the CLDN12 rs1017105 CC genotype, 9.8% in patients with the CT genotype and 28.6% in patients with the TT genotype. In the univariate and multivariate analyses, no significant differences were detected in the genotypes of rs1017105 between the pCR and non-pCR patients. Further analysis revealed significant differences in rs1017105 between the pCR and non-pCR patients with luminal-type BC (Table 4). The genotype distributions in the pCR and non-pCR patients with luminal-type BC are shown in Table 4. In the recessive model, women carrying the TT (OR =5.80, 95% CI: 1.02–23.49, P=0.014) genotype of CLDN12 rs1017105 had a higher pCR rate than those carrying the CC + CT genotypes (Table 4), which suggests that the genotypes of rs1017105 are associated with response to neoadjuvant chemotherapy.
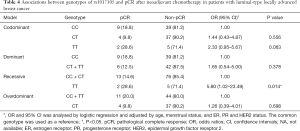
Full table
Discussion
To our knowledge, this is the first study that has investigated mirSNPs that potentially affect miRNA let-7 binding to the HIF1AN and CLDN12 genes and that has revealed their impact on pathologic response to taxane- and platinum-based neoadjuvant chemotherapy in BC. In this translational study, we found for the first time that SNPs in miRNA let-7-related genes (rs11292 located in the HIF1AN gene and rs1017105 located in the CLDN12 gene) could predict pCR to taxane- and platinum-based neoadjuvant chemotherapy in LABC. In the neoadjuvant setting, it is important to identify non-responders to avoid ineffective treatments and to provide alternative therapies such as surgery or switching to a non-cross resistant chemotherapy regimen.
In this study, our data showed that HIF1AN rs11292, a let-7 mirSNP, could predict pathologic complete response to taxane- and platinum-based neoadjuvant chemotherapy in BC. Saridaki et al. found that a let-7 miRNA binding site polymorphism in KRAS predicts improved outcome in patients with metastatic colorectal cancer who are treated with salvage cetuximab/panitumumab monotherapy (21). The impact of miRSNPs in the HIF1AN gene on the efficacy of neoadjuvant chemotherapy has not previously tested. Zheng et al. found that body fat possibly plays an important role in the development of BC and that this risk might be modified by specific genotypes of some potential genes including the HIF1AN gene (30). The results of our study and others are consistent, which suggests that genetic variations in miRNA let-7 binding sites in the HIF1AN gene may modulate the signalling response and the maintenance of genomic stability; this ultimately affects the efficacy of chemotherapy.
We demonstrated that CLDN12 rs1017105 could predict pathologic complete response to taxane- and platinum-based neoadjuvant chemotherapy in women with luminal-type BC. Hansen et al. hypothesized that the characterization of taxane resistance-associated molecular alterations and the identification and validation of putative predictive markers will have the potential to result in more effective use of taxanes, with improved survival and reduced toxicities and costs. In their study, the use of human BC cell lines grown in vitro allowed for the investigation of genomic alterations during multiple steps in the process towards a docetaxel-resistant phenotype. Additionally, they showed that MCF-7 cells acquired several copy number gains in chromosome 7, including in the ABCB1, ABCB4 and CLDN12 genes (31). Yang et al. investigated the relationship between claudins and IL-18. They showed that exogenous IL-18 enhanced BC cell migration and suppressed the expression of the tight junction proteins claudin-1, claudin-3, claudin-4 and claudin-12 in MCF-7 cells (32). The knockdown of claudin-3, claudin-4, and claudin-12 increased BC cell migration with maximal effects observed in claudin-12 siRNA-transfected cells. Their results suggest that IL-18 is an important factor for the induction of BC cell migration through downregulation of claudin-12. Taken together, these results align with our findings. Therefore, SNPs of miRNA let-7-related gene networks may serve as predictive biomarkers of taxane- and platinum-based neoadjuvant chemotherapy in luminal-type BC.
The present study has some limitations. The sample size of the patient cohort was small. Our findings indicated that SNPs of let-7-related genes (rs11292 located in the HIF1AN gene and rs1017105 located in the CLDN12 gene) were associated with response to neoadjuvant chemotherapy and had a potential role as predictive markers in a clinical setting. However, we admit that we did not investigate the underlying molecular mechanisms.
In conclusion, the results of the present study showed that miRNA let-7 binding site genetic variants located in the HIF1AN and CLDN12 genes could predict pCR to taxane- and platinum-based neoadjuvant chemotherapy in LABC. However, further work is needed to clarify the underlying molecular mechanisms.
Acknowledgments
Funding: The research is supported by grants from the National Natural Science Foundation of China (grant numbers 81172505 and 81302302), the Nurturing Fund of Renji Hospital 2016 (grant number PYMDT-002) and the Nurturing Fund of Renji Hospital 2015 (grant number RJZZ15-023). The funders had no role in study design, data collection and analysis, decision to publish, or preparation of the manuscript.
Footnote
Conflicts of Interest: The authors have no conflicts of interest to declare.
Ethical Statement: This study was conducted in accordance with the Declaration of Helsinki. Informed consent for participation in the study or use of their tissue was obtained from all participants. Each patient provided written informed consent for the publication of any associated data and accompanying images.
References
- Esquela-Kerscher A, Slack FJ. Oncomirs - microRNAs with a role in cancer. Nat Rev Cancer 2006;6:259-69. [Crossref] [PubMed]
- Al-Khanbashi M, Al-Moundhri M.. Micro-Ribonucleic Acid and Carcinogenesis: Breast Cancer as an Example. Oncol Rev 2015;9:279. [Crossref] [PubMed]
- Fabris L, Ceder Y, Chinnaiyan AM, et al. The Potential of MicroRNAs as Prostate Cancer Biomarkers. Eur Urol 2016;70:312-22. [Crossref] [PubMed]
- Cekaite L, Eide PW, Lind GE, et al. MicroRNAs as growth regulators, their function and biomarker status in colorectal cancer. Oncotarget 2016;7:6476-505. [Crossref] [PubMed]
- Johnson SM, Grosshans H, Shingara J, et al. RAS is regulated by the let-7 microRNA family. Cell 2005;120:635-47. [Crossref] [PubMed]
- Sampson VB, Rong NH, Han J, et al. MicroRNA let-7a down-regulates MYC and reverts MYC-induced growth in Burkitt lymphoma cells. Cancer Res 2007;67:9762-70. [Crossref] [PubMed]
- Lee YS, Dutta A. The tumor suppressor microRNA let-7 represses the HMGA2 oncogene. Genes Dev 2007;21:1025-30. [Crossref] [PubMed]
- Wu J, Li S, Jia W, et al. Reduced Let-7a Is Associated with Chemoresistance in Primary Breast Cancer. PLoS One 2015;10:e0133643. [Crossref] [PubMed]
- Dias K, Dvorkin-Gheva A, Hallett RM, et al. Claudin-Low Breast Cancer; Clinical & Pathological Characteristics. PLoS One 2017;12:e0168669. [Crossref] [PubMed]
- Geretto M, Pulliero A, Rosano C, et al. Resistance to cancer chemotherapeutic drugs is determined by pivotal microRNA regulators. Am J Cancer Res 2017;7:1350-71. [PubMed]
- Yang X, Cai H, Liang Y, et al. Inhibition of c-Myc by let-7b mimic reverses mutidrug resistance in gastric cancer cells. Oncol Rep 2015;33:1723-30. [Crossref] [PubMed]
- Xiang Q, Tang H, Yu J, et al. MicroRNA-98 sensitizes cisplatin-resistant human lung adenocarcinoma cells by up-regulation of HMGA2. Pharmazie 2013;68:274-81. [PubMed]
- Kaufmann M, von Minckwitz G, Mamounas EP, et al. Recommendations from an international consensus conference on the current status and future of neoadjuvant systemic therapy in primary breast cancer. Ann Surg Oncol 2012;19:1508-16. [Crossref] [PubMed]
- van der Hage JA, van de Velde CJ, Julien JP, et al. Preoperative chemotherapy in primary operable breast cancer: results from the European Organization for Research and Treatment of Cancer trial 10902. J Clin Oncol 2001;19:4224-37. [Crossref] [PubMed]
- Mauri D, Pavlidis N, Ioannidis JP. Neoadjuvant versus adjuvant systemic treatment in breast cancer: a meta-analysis. J Natl Cancer Inst 2005;97:188-94. [Crossref] [PubMed]
- Liedtke C, Mazouni C, Hess KR, et al. Response to neoadjuvant therapy and long-term survival in patients with triple-negative breast cancer. J Clin Oncol 2008;26:1275-81. [Crossref] [PubMed]
- Rastogi P, Anderson SJ, Bear HD, et al. Preoperative chemotherapy: updates of National Surgical Adjuvant Breast and Bowel Project Protocols B-18 and B-27. J Clin Oncol 2008;26:778-85. [Crossref] [PubMed]
- Guarneri V, Broglio K, Kau SW, et al. Prognostic value of pathologic complete response after primary chemotherapy in relation to hormone receptor status and other factors. J Clin Oncol 2006;24:1037-44. [Crossref] [PubMed]
- Cortazar P, Zhang L, Untch M, et al. Pathological complete response and long-term clinical benefit in breast cancer: the CTNeoBC pooled analysis. Lancet 2014;384:164-72. [Crossref] [PubMed]
- He L, Thomson JM, Hemann MT, et al. A microRNA polycistron as a potential human oncogene. Nature 2005;435:828-33. [Crossref] [PubMed]
- Saridaki Z, Weidhaas JB, Lenz HJ, et al. A let-7 microRNA-binding site polymorphism in KRAS predicts improved outcome in patients with metastatic colorectal cancer treated with salvage cetuximab/panitumumab monotherapy. Clin Cancer Res 2014;20:4499-510. [Crossref] [PubMed]
- Geng JQ, Wang XC, Li LF, et al. MicroRNA-related single-nucleotide polymorphism of XPO5 is strongly correlated with the prognosis and chemotherapy response in advanced non-small-cell lung cancer patients. Tumour Biol 2016;37:2257-65. [Crossref] [PubMed]
- Permuth-Wey J, Fulp WJ, Reid BM, et al. STAT3 polymorphisms may predict an unfavorable response to first-line platinum-based therapy for women with advanced serous epithelial ovarian cancer. Int J Cancer 2016;138:612-9. [Crossref] [PubMed]
- Pardini B, Rosa F, Barone E, et al. Variation within 3'-UTRs of base excision repair genes and response to therapy in colorectal cancer patients: A potential modulation of microRNAs binding. Clin Cancer Res 2013;19:6044-56. [Crossref] [PubMed]
- Mahon PC, Hirota K, Semenza GL. FIH-1: a novel protein that interacts with HIF-1alpha and VHL to mediate repression of HIF-1 transcriptional activity. Genes Dev 2001;15:2675-86. [Crossref] [PubMed]
- Hameiri-Grossman M, Porat-Klein A, Yaniv I, et al. The association between let-7, RAS and HIF-1alpha in Ewing Sarcoma tumor growth. Oncotarget 2015;6:33834-48. [Crossref] [PubMed]
- Ouban A, Ahmed AA. Claudins in human cancer: a review. Histol Histopathol 2010;25:83-90. [PubMed]
- Tan EY, Campo L, Han C, et al. Cytoplasmic location of factor-inhibiting hypoxia-inducible factor is associated with an enhanced hypoxic response and a shorter survival in invasive breast cancer. Breast Cancer Res 2007;9:R89. [Crossref] [PubMed]
- Zhou L, Xu S, Yin W, et al. Weekly paclitaxel and cisplatin as neoadjuvant chemotherapy with locally advanced breast cancer: a prospective, single arm, phase II study. Oncotarget 2017;8:79305-14. [PubMed]
- Zhu Z, Teng Z, van Duijnhoven FJ, et al. Interactions between RASA2, CADM1, HIF1AN gene polymorphisms and body fatness with breast cancer: a population-based case-control study in China. Oncotarget 2017;8:98258-69. [Crossref] [PubMed]
- Hansen SN, Ehlers NS, Zhu S, et al. The stepwise evolution of the exome during acquisition of docetaxel resistance in breast cancer cells. BMC Genomics 2016;17:442. [Crossref] [PubMed]
- Yang Y, Cheon S, Jung MK, et al. Interleukin-18 enhances breast cancer cell migration via down-regulation of claudin-12 and induction of the p38 MAPK pathway. Biochem Biophys Res Commun 2015;459:379-86. [Crossref] [PubMed]


