
Hemorrhagic bulla: a rare presentation of scabies
Introduction
The typical symptom of scabies is an intense, intractable, generalized pruritus that is worse at night (1-8). The most common presentations of scabies include classic burrows, pruritic papules, and inflammatory nodules (1-8). In rare conditions, the lesions of scabies may mimic that of impetigo, psoriasis, contact dermatitis, urticaria, Darier’s disease, or dermatitis herpetiformis (1,2); and may even present as bullous lesions masquerading as bullous pemphigoid, called bullous scabies (1-6). Up to date, about 50 cases of bullous scabies have been reported (1-9). Although bullous scabies associated with hemorrhage was mentioned in the literature (2), to our knowledge, no case of scabies associated with hemorrhagic bulla has been described to date. Herein, we report a 90-year-old man of scabies hospitalized in the ward with associated hemorrhagic bullae on both his feet and hands.
Case presentation
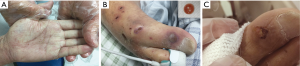
A 90-year-old man, hospitalized in intensive care unit, complained of generalized itching papules and blisters for 2-month duration. The lesions had been increasing in numbers slowly since its first occurring, that were contagious and had poor responses to systemic antihistamines and sodium thiosulfate as well as topical steroids. The patient had been bedridden for years because of bad conditions. Before the itching lesions occurred, he had been treated with antibiotics and palliative managements because of anemia, pneumonia and pleural effusion. Other significant past medical histories included hypertension, cerebral infarction, depression, vascular dementia. Some individuals in close contact with the patient, including one of his daughters and an attendant, and some patients in the intensive care unit, presented similar itching papules on their trunk and limbs in sequence after the patient’s occurrence, however, they were absent for bulla as well as hemorrhagic lesions. Cutaneous examination showed that generalized discrete papules, papulovesicle and nodules distributed over the patient’s whole-body surface except his scalp and face, with predilection for distal extremities (Figure 1A) and trunk. Multiple, isolated intact tense bullae, filled with bloody fluid and with erythema around, measuring approximately 0.5 to 1 cm in diameter, as well as excoriations were also noted on the dorsal aspects of both feet (Figure 1B) and hands, with negative Nikolsky sign over the lesions. The mucosae were not involved. After the bullae were punctured with a needle, bloody fluid (Figure 1B, the inset) discharged that was negatively cultured for bacteria and fungi as well as absent for scabies egg or mite by smearing. Scraping the papular lesions on the trunk revealed both mites and eggs of Sarcoptes Scabiei. Skin biopsy was refused. The patient was diagnosed with scabies associated with hemorrhagic bullae, and was treated with topical 10% sulfur ointment alone, twice daily for 3 days, leading to a rapid remission of the papules and papulovesicle, after treatment for 3 cycles. Finally, the bullae cured slowly without scars leaving behind (Figure 1C). All other scabies sufferers including his daughter and the patients in the unit were cured by topical 10% sulfur ointment. The patient remained lesions free for up to more than 9 months of follow-up.
Discussion
Based on the typical lesions, the contagiousness of lesions, the detection of mites and response to medication, the diagnosis of scabies for the present patient could be confirmed. Scabies is a common, worldwide, infectious cutaneous disease, which affects the individuals of all ages, and socio-economic classes in any climate regions, it has a preference for the young without any gender difference and racial predominance (1-8). Bullous scabies is a rare subtype of scabies with a male predilection which commonly affects the elderly with a median age of 70 years old although it has been reported involving the individuals from 1 to 89 years old (1-9). To our knowledge, only eight cases have been reported younger than 10 years old (1-3,9). The lesions of bullous scabies usually present as intensely pruritic bullae, which may be tense or flaccid and at times may have associated hemorrhage (2), and mainly distribute on arms, legs and trunk, and less on feet (1-4,6,9). It is notable that the present patient was 90 years old, and all the bullae were hemorrhagic and distributed over the distal extremities, to our knowledge, no similar conditions have been reported previously. Although the exact morbidity rate of hemorrhagic bulla on scabies remains unknown, we considered that hemorrhagic bulla is indeed an exceptionally rare presentation for scabies in consideration of rare report of bullous scabies.
The common risk factors for scabies include overcrowding, immigration, poor hygiene, poor nutritional status, homelessness, dementia, sexual or close contact, and sometimes, immunosuppression is also the triggering factor (1,7,8). The present patient had poor conditions and was in bedridden status, which, we considered, might be responsible for the infection of scabies.
The mechanisms of bullous formation in scabies are not entirely clear, although autoeczematization, superinfection, the direct injury or secretion of lytic enzymes by the scabies mites, and cross-reactivity of scabies protein with basal membrane zone antigens are considered to be the possible pathogenesis of bullous scabies (1-6). As the bullae were surrounded by erythema and no bullae were present during the follow-up, the most possibility for the formation of hemorrhagic bullae of present patient, we considered, is that it may be caused by the infection of scabies itself rather than by the itching-induced friction, although we cannot absolutely exclude the possibility that itching-induced friction might play role for the bullous formation. Because all the other patients in the ward presented scabies after contacted this patient, the present patient could be considered the source of infection. However, all other patients were absent for bullous and hemorrhagic lesions, this phenomenon demonstrates that scabies-induced bullae are only related to the patient individuals but not to scabies itself (3).
The differential diagnosis of bullous scabies includes pemphigus, bullous pemphigoid, insect bite reaction, bullous impetigo, and acquired epidermolysis bullosa, etc. (1-6). As the patient of scabies presents itching papules which are contagious and have good response to antiscabietics, it is not difficult to make a correct diagnosis. Dermoscope may be a rapid and noninvasive tool for the diagnosis of scabies, because it can help us to detect the burrows, scabies mites or eggs in the skin that are not visible by the naked eye (10). Based on the response to the treatment for the present patient, we supported the opinions that antiscabietics, including systemic and topical treatments, are the optimal options for all the bullous scabies (1-5), although the mechanism of formation of bullae in bullous scabies is considered to be immune mediated and it is still hard to explain why such a condition occurs (5).
The case we reported demonstrated that scabies may present as hemorrhagic bulla atypically and cause nosocomial infection.
Acknowledgements
The authors sincerely thank the patient participating the present work.
Footnote
Conflicts of Interest: The authors have no conflicts of interest to declare.
Informed Consent: Written informed consent was obtained from the legal guardians of the patient for publication of the present manuscript and any accompanying images.
References
- Luo DQ, Huang MX, Liu JH, et al. Bullous Scabies. Am J Trop Med Hyg 2016;95:689-93. [Crossref] [PubMed]
- Maan MA, Maan MS, Sohail AM, et al. Bullous scabies: a case report and review of the literature. BMC Res Notes 2015;8:254. [Crossref] [PubMed]
- Luo ZY, Zeng M, Gao Q, et al. Case Report: Bullous Scabies in Two Children below 10 Years. Am J Trop Med Hyg 2017;97:1746-8. [Crossref] [PubMed]
- Serra D, Pedro Reis J, Mariano A, et al. Recurrent bullous scabies. J Cutan Med Surg 2010;14:175-7. [Crossref] [PubMed]
- Chen MC, Luo DQ. Bullous scabies failing to respond to glucocorticoids, immunoglobulin, and cyclophosphamide. Int J Dermatol 2014;53:e265-6. [Crossref] [PubMed]
- Cohen PR. Scabies masquerading as bullous pemphigoid: scabies surrepticius. Clin Cosmet Investig Dermatol 2017;10:317-24. [Crossref] [PubMed]
- Hengge UR, Currie BJ, Jäger G, et al. Scabies: a ubiquitous neglected skin disease. Lancet Infect Dis 2006;6:769-79. [Crossref] [PubMed]
- Hicks MI, Elston DM. Scabies. Dermatol Ther 2009;22:279-92. [Crossref] [PubMed]
- Wang AL, Rainwater YB, Mauskar MM. Bullous eruption in 2 brothers. Cutis 2018;101:169;178.
- Park JH, Kim CW, Kim SS. The diagnostic accuracy of dermoscopy for scabies. Ann Dermatol 2012;24:194-9. [Crossref] [PubMed]


