Frailty in elderly ICU patients in Greece: a prospective, observational study
Introduction
In recent years, several studies have been conducted on the onset of frailty syndrome in older patients (referrals). It has been observed that such individuals have features such as weight loss and muscle mass, change in their eating habits, movement and endurance, impairment of their mental function, which makes them more prone to adverse health outcomes. Perhaps these characteristics may be the reason why there has been a marked increase in hospitalization in ICU in Greece by the elderly (1-5).
The frailty syndrome is closely related to the mental state of the sufferers. Surveys conducted in the community have shown that individuals characterized as weak have multiple mental deficits that indicate disability and are related or caused by both endogenous and environmental factors. Approximately at the age of 70 years, a significant percentage has been observed to have mild cognitive decline and another percentage of dementia. The age and cessation of cognitive function are two events interrelated and not randomly linked to each other. At the end of time, lesions at the cellular and molecular levels accumulate and become visible in the form of diseases (2,6,7).
The state of the patient’s health as determined by the biological characteristics rather than the chronological age prior to admission, provides information on the patient’s progress in the ICU and the probability of mortality. Knowing the needs and deficits of each patient individually, it is possible to create a care plan suitable to cover all the patient’s needs. This assessment of the baseline functional situation and the burden posed by pre-existing illness have a predictive value and are an important criterion in assessing a patient who needs intensive care (1).
Based on the foregoing, it is understandable that the nature of the syndrome is a challenge in formulating its definition. Frailty extends beyond deficits (functional limitation) and coexisting illnesses and recognizes that a patient can be sick without being weak or vice versa. Aging is influenced by both the genetic background and the environment and begins from the embryonic period. The mechanisms that determine the aging process as soon as they become clear. Recognizing that aging is a heterogeneous process, many doctors are looking for a method to quantify biological age rather than just chronological age. Since frailty syndrome is directly related to the aging process, it is assumed that this syndrome is measurable (1,4).
The purpose of the study was the prevalence of frailty syndrome in subjects aged 65 years who were hospitalized in an intensive care unit in Greece.
Methods
This is a prospective, observational study by investigating groups of patients who differ in the stage of development of the frailty syndrome. The sample of the study consisted of the families or carers of 36 patients hospitalized in ICU. Patient selection criteria were over 65 years of age and have 1 to 5 criteria for controlling the phenotype. The study was conducted in a General Hospital in Greece over a period of 1 year (01/06/2016–01/06/2017). The simple random sampling method was chosen to collect the sample. The CSHA Clinical Frailty Scale (CFS) consisting of 7 levels was used and was answered by the patient’s family or carer. It was preceded by a 5-criterion frailty phenotype test, so that the patient, depending on the number of criteria he had, would fall into one of three categories: positive frailty syndrome, pre-developmental stage and negative (absence of criteria). In addition, the severity of the patients with APACHE II (Acute Physiology and Chronic Health Assessment), SAPS II (Simplified Acute Physiology) and SOFA (Sequential Organ Failure Assay) were assessed, and all possible correlations were made (8).
Statistical analysis
For the analysis of the data was used the SPSS 19 for windows statistical package and more specifically descriptive statistics and correlations with parametric methods.
Results
The sample of the study
Thirty-six heavy patients who were admitted to the ICU General Hospital of the Prefecture of Attica, aged 65 years and older, were studied. The female population amounted to 22 and the male to 14. The other demographic and other data are shown in Table 1.
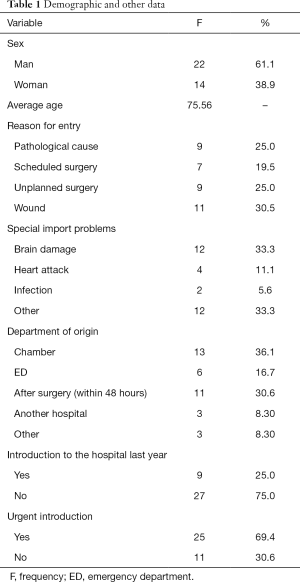
Full table
In 36 patients the gravity of their condition was assessed with APACHE, SAPS II, SOFA (24, 48, 92 h) and Glasgow scales. In addition, McCabe’s life expectancy was used, co-occurring Charlson diseases, as well as memory disorders. In particular the effects of phenotype frailty, and CFS (Table 2), were tested.
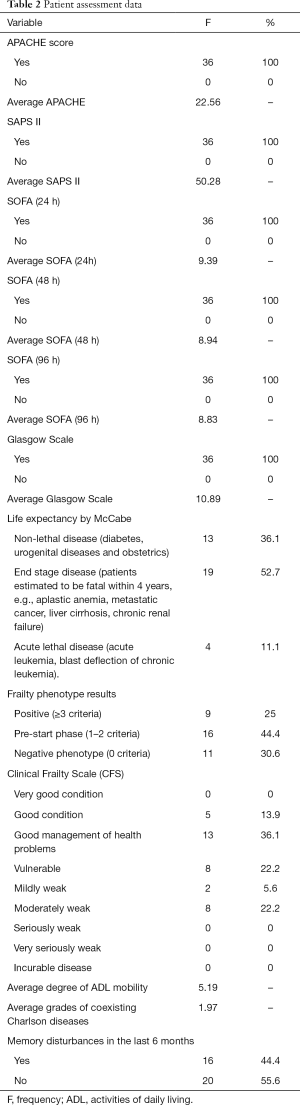
Full table
In the framework of the present study, the basic elements of patient hospitalization were recorded (Table 3).
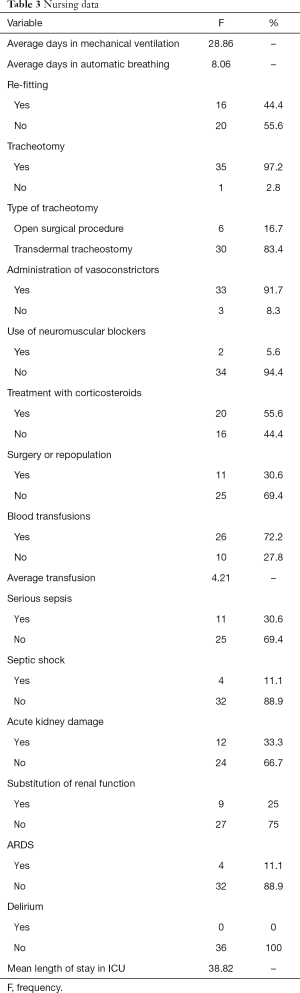
Full table
The course of patient health after hospitalization in the ICU was recorded, as well as mortality rates (Table 4).
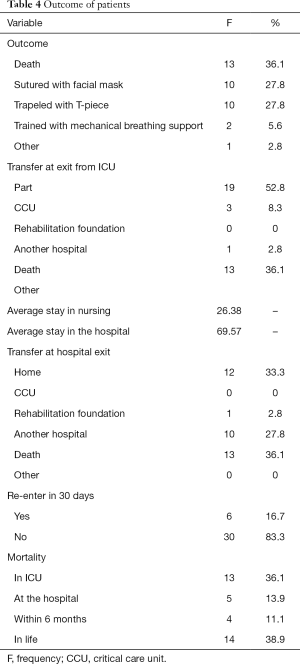
Full table
CFS correlation and determinants
A significant correlation between the CFS scale and APACHE (P=0.041), age (P=0.033), sex (P=0.049) and activities of daily living (ADL) mobility index (P=0.001) was found to be significant. In contrast, no correlation was found between CFS and memory impairment (P=0.910) and the Glasgow scale (P=0.713).
Discussion
The 36 patients were categorized based on the phenotype of frailty, which separates them into positive and negative, but also takes into account the individuals who are in the pre-stage of the onset of the syndrome. Thus, 25% of them seemed to collect over 3 features. 44.4% were at an early stage of the syndrome with 1–2 characteristics, while 30.6% had no symptoms. Similarly, in France, of the 961 patients enrolled in the ICU, 73.3% of the subjects were not weak, while 26.7% were found to be weak. 20.3% of them had 3 or more characteristics and 79.7% had 1 or 2 characteristics. In both cases these people were ranked high in the CFS scale (5).
The age limit of this study was similar to the criterion in French and Canadian research. The study, which took place in a hospital in Brisbane, Australia, was composed of 110 patients of the same age category (5). The collection of information so far has been done by the patients themselves in the Canadian and Australian research, and due to the nature of the ICU hospitals, for the French research, and for the present survey the information was collected from the close family environment (4,9,10).
For a clearer determination of health status, scales that are easy to use in ICUs such as SAPS II, SOFA, APACHE and the Glasgow scale were used in the present study, as was done in the French survey, except that they were not taken take into account the SOFA results of the first three twenty-four hours as was the case in the current survey. In both cases the results were useful as prognostic tools (5).
Significant correlation in French research on the scale of inability to determine the degree of ADL mobility. Particularly, the distribution of patients who proved to be weak, have common characteristics with those with low mobility (11-13). Results similar to this survey.
A significant role is played by memory disorders, where the rate of this research is positive in 44.4% of the severely ill patients. In the French survey the incidence of these disorders is 43%. The incidence of cognitive impairment in Canadian research is 39.7%. In addition to the Australian survey, the discount rate is at 20% (5,9,10).
In addition to the above features, which are related to patient assessment, with the onset of frailty syndrome, their stay and hospitalization are important. In particular, in this research and in French research, the causes of admission were segregated into pathological causes, planned surgeries, unscheduled surgical interventions and the cause of trauma. In our own research, the proportion of patients admitted with pathological causes was 25%, while in France 50%. Scheduled surgical interventions amounted to 19.5% of the sample and 52% to France. The proportion of people who have undergone unplanned surgery has reached 25% and at the same time France in 72%. Wounding accounted for 30.5% of the current survey, while in France only 18%. Additionally, special import problems such as brain injury, cardiac arrest or a serious infection in the two investigations (5) play an important role.
In addition, hospitalization in the ICU was significantly significant, during which the average mechanical ventilation was recorded (28.86 days), while in France the average days were 11. Neuromuscular blockade was used on average at 5.6% France were granted 24%. Corticosteroids were used at 55.6% in our own research and in France research 43% respectively. During hospitalization, 30.6% of our patients experienced severe sepsis, while the ICU of the French Hospital accounted for 37% (5).
In all the above, an attempt was made to relate the length of hospitalization to the ICU, where our patients stayed for an average of 38.82 days while the stay in the ICU of France lasted about 8 days. The total stay in the Greek hospital averages 69.57 days, while on average the days of hospitalization are on average 33.99 days (5).
Finally, what was considered was the viability and mortality of the severely ill patients, both within the ICU and 6 months after their discharge. In the present study 36.1% of patients died in the ICU, 11.1% died within the next 6 months and 38.9% were alive. Respectively, in the ICU of France these percentages were 23.03%, 56% and 20.97% respectively. The Canadian survey set the mortality study as a plan up to 5 years after leaving the hospital for this and its results are not compared with the above data. It is therefore assumed that the prognosis of the syndrome of frailty is carried out at various levels taking into account a variety of information on the health condition of the patient before and at the time of import, and draws conclusions about his/her outcomes until and after leaving the hospital (5,9).
Conclusions
The findings of the study highlighted the onset of frailty syndrome in ICU patients. The objective assessment of the frailty syndrome in the severely ill patient provides a clearer picture of its out-of-hospital condition and contributes to the collection of information on the outcomes of the inpatient. In attempts to quantify and measure the frailty that have been done so far, a tool widely used mainly in surgery has been the frailty index. A questionnaire of seventy questions capable of detecting patient deficits, creating an image of individuals who are likely to have an adverse outcome on their introduction to the ICU. However, the Frailty Index alone is difficult to integrate into an ICU where work rates are intense and medical staff are dealing with heavy sufferers to the extent that detailed information is required. At the same time, estimation of predictive indicators such as APACHE II, SAPS II and SOFA is required.
Acknowledgements
None.
Footnote
Conflicts of Interest: The authors have no conflicts of interest to declare.
Ethical Statement: The ethical review board of our hospital approved this study (IRB# 2016-04).
References
- McDermid RC, Stelfox HT, Bagshaw SM. Frailty in the critically ill: a novel concept. Crit Care 2011;15:301. [Crossref] [PubMed]
- Soysal P, Stubbs B, Lucato P, et al. Corrigendum to “inflammation and frailty in the elderly: a systematic review and meta-analysis” Ageing Res Rev 2017;35:364-5. [Ageing Res Rev. 31 (2016) 1-8]. [Crossref] [PubMed]
- Searle SD, Rockwood K. Frailty and the risk of cognitive impairment. Alzheimers Res Ther 2015;7:54. [Crossref] [PubMed]
- Rockwood K, Theou O, Mitnitski A. What are frailty instruments for? Age Ageing 2015;44:545-7. [Crossref] [PubMed]
- Le Maguet P, Roquilly A, Lasocki S, et al. Prevalence and impact of frailty on mortality in elderly ICU patients: a prospective, multicenter, observational study. Intensive Care Med 2014;40:674-82. [PubMed]
- McMillan GJ, Hubbard RE. Frailty in older inpatients: what physicians need to know. QJM 2012;105:1059-65. [Crossref] [PubMed]
- Morley JE, Morris JC, Berg-Weger M, et al. Brain health: the importance of recognizing cognitive impairment. J Am Med Dir Assoc 2015;16:731-9. [Crossref] [PubMed]
- Strand K, Flaatten H. Severity scoring in the ICU: a review. Acta Anaesthesiol Scand 2008;52:467-78. [Crossref] [PubMed]
- Rockwood K, Song X, MacKnight C, et al. A global clinical measure of fitness and frailty in elderly people. CMAJ 2005;173:489-95. [Crossref] [PubMed]
- McRae PJ, Walker PJ, Peel NM, et al. Frailty and geriatric syndromes in vascular surgical ward patients. Ann Vasc Surg 2016;35:9-18. [Crossref] [PubMed]
- Crocker T, Young J, Forster A, et al. The effect of physical rehabilitation on activities of daily living in older residents of long-term care facilities: systematic review with meta-analysis. Age Ageing 2013;42:682-8. [Crossref] [PubMed]
- Vermeulen J, Neysen JC, van Rossum E, et al. Predicting ADL disability in community-dwelling elderly people using physical frailty indicators: a systematic review. BMC Geriatr 2011;11:33. [Crossref] [PubMed]
- Fieo RA, Austin EJ, Starr JM, et al. Calibrating ADL-IADL scales to improve measurement accuracy and to extend the disability construct into the preclinical range: a systematic review. BMC Geriatr 2011;11:42. [Crossref] [PubMed]


