Improvement in hamstring and quadriceps muscle strength following cruciate-retaining single radius total knee arthroplasty
Introduction
Although total knee arthroplasty (TKA) have been shown to alleviate pain and improve function, a large percentage of patients remain dissatisfied after their procedure (1-3). In the current healthcare climate, patient satisfaction following this procedure has become further scrutinized. Despite improvements post-operatively, up to 20% of patients report persistent muscle weakness as the primary reason for their dissatisfaction (4,5).
Improvement in function following TKA is largely attributed to restoration of strength of the extensor mechanism of the knee (6) Following TKA, quadriceps and hamstring muscle strength weakness can persist for up to 2 years post-operatively, translating into difficulty with activities of daily living such as stair climbing or walking (7-12). However, gaining post-operative improvements in quadriceps and hamstring muscle strength can be multi-factorial. Several factors including age, body mass index (BMI), surgical technique, and implant design may play a role (13-15). A single-radius prosthesis has been designed to improve the functional recovery after TKA. This implant type proposes several advantages when compared to a multi-radius design. With only one flexion-extension axis, stability is sustained throughout movement, and it requires less recruitment of quadriceps strength compared to multi-radius designs to perform activities of daily living (16-19). Furthermore, compared to multi-radius designs, single radius (SR) implants have been shown to offer a quicker time to recover (16,20). It has been postulated that these designs may aid in improvements of muscle strength, range of motion (ROM), and potentially patient reported outcomes.
Currently there is a paucity of literature available describing the influence of patient characteristics, surgical factors, and clinical outcomes on quadriceps and hamstring muscle strength following TKA with a cruciate-retaining, SR implant. For this reason, we sought to investigate TKA patients for: (I) quadriceps muscle strength; (II) hamstring muscle strength; (III) flexion/extension (F/E) ratio; (IV) clinical outcome scores; (V) influence of patient characteristics on muscle strength at 1-year post-operatively.
Methods
Patient selection
Following Institutional Review Board approval, 41 patients (41 knees) undergoing primary TKA from February 1st, 2006 to July 31st, 2013 were prospectively enrolled to evaluate quadriceps and hamstring muscle strength. All procedures were performed by a single, fellowship trained adult reconstruction orthopaedic surgeon at a single, high-volume institution. The following patients were considered for inclusion: (I) functionally intact PCL; (II) less than 15 degrees of varus; (III) minimum of 1-year post-operative follow-up; (IV) treated with the Scorpio CR (Stryker Orthopaedics, Mahwah, New Jersey, USA) implant. Patients who had less than 1-year post-operative follow-up or incomplete isokinetic strength testing data were excluded [two patients (2 knees)]. Post-operative range of ROM measurements were missing from two patients and were excluded from this sub-group evaluation as well.
A total of 39 patients (39 knees) who completed 1-year follow-up were included for analysis. The cohort consisted of 13 women and 26 men, who had a mean age of 68 years (range, 51 to 88 years) and a mean BMI of 32 kg/m2 (range, 23 to 48 kg/m2). There were 21 patients (54%) who that reported contralateral knee (n=17, 43%), hip (n=1, 2%) or both (n=3, 8%) pathology or prior arthroplasty. Eleven patients (28%) reported concomitant back pathology including lumbar spinal stenosis, lumbar degenerative disc disease, and chronic lower back pain. One patient (2%) underwent a revision surgery prior to isokinetic testing and was excluded from the analysis. There were no post-operative complications.
Study design
All patients who underwent a TKA received spinal anesthesia with a proximal femoral block. The procedure was performed with a standard midline skin incision, utilizing a midvastus (19 patients) or subvastus (20 patients) approach. Following surgery, all patients were admitted and placed on a patient controlled analgesia (PCA) pump for the first 23 hours. Patients were given aspirin as venous thromboembolism (VTE) prophylaxis, along with intermittent pneumatic compression and early mobilization. Physical therapy began on the first postoperative day and continued for 6 to 12 sessions following discharge. All patients were discharged home within 48 hours of surgery.
Quadriceps and hamstring strength was assessed via an isokinetic dynamometer System 4 Pro (Biodex Medical Systems, Shirley, New York, USA) at the pre-operative and 1-year post-operative visit. Isokinetic dynamometer testing at 180 degree/second for 3 sets of 10 repetitions in extension and flexion was performed by an independent physical therapist to assess dynamic concentric torque of the hamstrings and quadriceps muscles. Clinical evaluations were performed using the Knee Society Score (KSS), as well as active ROM at pre-operative and 1-year post-operative (21).
Statistical analysis
All data was de-identified and imported into a Microsoft Excel (Excel; Microsoft, Redmond, Washington) spreadsheet. Statistical analyses were performed using SPSS Version 23 (IBM Corp., Armonk, New York, USA). Descriptive statistics were used to analyze the means and ranges for continuous variables. Comparisons of quadriceps and hamstrings muscle strength among groups were performed utilizing student t-tests. A P value of <0.05 was deemed statistically significant and 95% confidence intervals (CI) were used.
Results
Quadriceps strength
Mean quadriceps muscle strength significantly increased from pre-operative evaluation at 19 Nm/kg (SD 1; range, 5 to 36 Nm/kg) to post-operative evaluation at 23 Nm/kg (SD 8; range, 9 to 43 Nm/kg; P=0.0001, 95% CI: −6.088 to −2.625). The mean pre-to-post operative improvement was 4 Nm/kg (range, −4 to 20 Nm/kg) representing a 37% (range, –16% to 100%) increase in quadriceps muscle strength.
Hamstring strength
Mean hamstring muscle strength significantly improved from pre-operative evaluation at 15 Nm/kg (SD 6; range, 6 to 29 Nm/kg) to post-operative evaluation, 19 Nm/kg (SD 8; range, 8 to 37 Nm/kg; P=0.0433, 95% CI: −6.307 to −0.099). This represents a mean of 3 Nm/kg (range, −5 to 14) or 26% (range, −22% to 100%) increase in hamstring muscle strength.
Flexion/extension ratio
There was a decrease from pre-operative F/E ratio of 0.88 (SD 0.2; range, 0.5 to 1.3) to post-operative F/E ratio of 0.83 (SD 0.2; range, 0.5 to 1.3; P=0.0936, 95% CI: −0.009 to 0.112).
Clinical outcomes scores
The mean pre-operative ROM was 5 (SD 3) degrees of extension to 97 (SD 9) degrees of flexion. Mean post-operative ROM was 0 (SD 1) degrees of extension to 117 (SD 8) degrees of flexion. Pre-to-post operative mean ROM improvement was 5 degrees of extension (P=0.0001, 95% CI: 4.07 to 6.25) and 20 degrees of flexion (P=0.0001, 95% CI: −23.51 to −16.39).
The mean KSS pain was 95 points (SD 4, range, 84 to 100 points) postoperatively and mean KSS function was 96 points (SD 6, range, 80 to 100 points) postoperatively.
Influence of demographics
Patients under the age of 65 years had significantly higher quadriceps muscle strength (26 vs. 21 Nm/kg, P=0.0443), and significantly higher hamstring muscle strength (22 vs. 16 Nm/kg, P=0.0092) post-operatively. However, no significant differences were noted in hamstring muscle strength (P=0.0837) or quadriceps muscle strength (P=0.0843) from pre-to-post operative based upon age (Table 1).
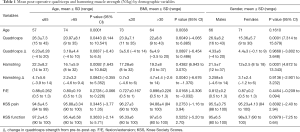
Full table
Male patients demonstrated greater post-operative extension and flexion strength than females (P=0.0001), however, there was no difference in pre-to-postoperative change in strength for extension or flexion based on gender (P=0.9668 for extension and P=0.9136 for flexion) (Table 1).
Sub-group analysis of BMI demonstrated that patients who had a BMI of >30 kg/m2 had a significantly higher pre-to post-operative gain in flexion strength (P=0.0040, 95% CI: −6.676 to −1.370). Furthermore, patients with BMI >30 kg/m2 had significantly higher post-operative F/E ratio compared to patients ≤30 kg/m2 (P=0.0168, 95% CI: −0.306 to −0.032).
The presence of concomitant back pathology, contralateral knee or hip pathology, or incision type did not influence post-operative quadriceps or hamstring muscle strength. However, patients who had contralateral hip or knee pathology demonstrated a higher post-operative F/E ratio, KSS function, and KSS pain scores (Table 2).
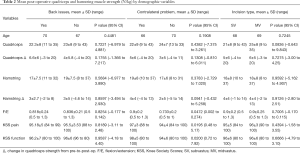
Full table
Discussion
Restoration of quadriceps and hamstring muscle strength following TKA is an important predictor of functional improvement and ultimately satisfaction following TKA (6). Previously, literature has demonstrated that restoration of strength can take as long as 2 years post-operatively to improve, thus presenting substantial disability to perform tasks of daily living (7-12). A single-radius design prosthesis offers several theoretical advantages in restoring post-operative quadriceps and hamstring muscle strength, however, there is a paucity of data investigating the influence of patient characteristics on muscle strength in the setting of a SR TKA. We demonstrated that patients who underwent TKA utilizing a SR, CR prosthesis had a 37% and 26% increase in quadriceps and hamstring muscle strength, had excellent ROM and KSS (95 to 96 points), while maintaining an appropriate F/E ratio. In addition, we found that patients who had a BMI of >30 kg/m2 had significantly higher gains in muscle strength from before to after surgery.
This study has several limitations. The relatively small sample size and sub-groups makes our results hard to extrapolate to the general public. Furthermore, only pre-to post-operative quadriceps and hamstring muscle strengths were evaluated with no comparison to an age-matched cohort or contralateral knee. Nevertheless, we were able to demonstrate excellent strength and functional outcomes in patients who received cruciate-retaining SR total knee arthroplasties.
Gómez-Barrena et al. evaluated isokinetic strength at 60 degrees/second in a case-control of 30 single radius (SR-Scorpio Stryker Orthopaedics, Mahwah, New Jersey) and 30 multi radius (MR-NexGen Simmer, Warsaw, Indiana) design TKA, demonstrating lower F/E ratio, increased extension peak torque (77 vs. 69), and decreased flexion peak torque (40 vs. 49) in the SR cohort. Furthermore, patients with SR design required fewer physical therapy session and were able to remove one crutches at a mean 1.5 weeks sooner (22). Biomechanical studies investigating the single-radius design have concluded that a more posterior flexion-extension access acts to lengthen the quadriceps moment arm and making the quadriceps more efficient (16,20). Alterations in movement mechanics as a compensatory effect of quadriceps and hamstring weakness decreased during sit-to-stand, stair climbing, or walking in patients post-operatively (10). Mahoney et al. performed a case-control study of independent rise from chair in 83 MR and 101 SR knees. At 1 year post-operatively 89% of patients within the SR group could independently rise from a chair compared to 74% of the multi-radius group (20). Furthermore, Wang et al. demonstrated that MR TKA design was associated with a higher degree of compensatory changes requiring a greater activation of the quadriceps and hamstring muscles during sit-to-stand movements (18). Similarly, Colwell et al. investigated 94 knees utilizing the Scorpio non-restrictive geometry-CR knee prosthesis, demonstrating at 1-year post-operatively 67% of knees had improved flexion and a mean flexion of 116.9 degrees (23). Conversely, Hall et al. compared 50 patients with Scorpio-PS and 50 patients with Press Fit Condylar Sigma design (Johnson & Johnson PFC; DePuy, Johnson & Johnson, Warsaw, Ind) demonstrating no difference in mean maximum flexion, with both cohorts at 106 (24). Nevertheless, most studies, including the present one, have demonstrated excellent outcomes with the use of SR, CR total knee arthroplasty design.
In conclusion, the use of a SR, CR total knee arthroplasty system provides significant improvements post-operatively in quadriceps and hamstring strength regardless of gender, age, contralateral knee pathology, back pathology, or incision type. Obese patients should be counseled that muscle weakness may persist post-operatively and appropriate pre-operative counseling on weight management is appropriate. Further comparative investigation on the impact of implant design on hamstring and quadriceps muscle strength is warranted. However, SR, CR total knee arthroplasty system demonstrated excellent results in terms of muscle strength and ROM improvements.
Acknowledgements
None.
Footnote
Conflicts of Interest: The authors have no conflicts of interest to declare.
Ethical Statement: The study was approved by Institutional Review Board of Bonutti Clinic.
References
- Carr AJ, Robertsson O, Graves S, et al. Knee replacement. Lancet 2012;379:1331-40. [Crossref] [PubMed]
- Hawker G, Wright J, Coyte P, et al. Health-related quality of life after knee replacement. J Bone Joint Surg Am 1998;80:163-73. [Crossref] [PubMed]
- Matsuda S, Kawahara S, Okazaki K, et al. Postoperative alignment and ROM affect patient satisfaction after TKA. Clin Orthop Relat Res 2013;471:127-33. [Crossref] [PubMed]
- Bourne RB, Chesworth BM, Davis AM, et al. Patient satisfaction after total knee arthroplasty: who is satisfied and who is not? Clin Orthop Relat Res 2010;468:57-63. [Crossref] [PubMed]
- Noble PC, Conditt MA, Cook KF, et al. The John Insall Award: patient expectations affect satisfaction with total knee arthroplasty. Clin Orthop Relat Res 2006.35-43. [Crossref] [PubMed]
- Sharma L, Dunlop DD, Cahue S, et al. Quadriceps strength and osteoarthritis progression in malaligned and lax knees. Ann Intern Med 2003;138:613-9. [Crossref] [PubMed]
- Rossi MD, Brown LE, Whitehurst M. Early strength response of the knee extensors during eight weeks of resistive training after unilateral total knee arthroplasty. J Strength Cond Res 2005;19:944-9. [PubMed]
- Silva M, Shepherd EF, Jackson WO, et al. Knee strength after total knee arthroplasty. J Arthroplasty 2003;18:605-11. [Crossref] [PubMed]
- Bjerke J, Öhberg F, Nilsson KG, et al. Peak knee flexion angles during stair descent in TKA patients. J Arthroplasty 2014;29:707-11. [Crossref] [PubMed]
- Mizner RL, Snyder-Mackler L. Altered loading during walking and sit-to-stand is affected by quadriceps weakness after total knee arthroplasty. J Orthop Res 2005;23:1083-90. [Crossref] [PubMed]
- Walsh M, Woodhouse LJ, Thomas SG, et al. Physical impairments and functional limitations: a comparison of individuals 1 year after total knee arthroplasty with control subjects. Phys Ther 1998;78:248-58. [Crossref] [PubMed]
- Casartelli NC, Item-Glatthorn JF, Bizzini M, et al. Differences in gait characteristics between total hip, knee, and ankle arthroplasty patients: a six-month postoperative comparison. BMC Musculoskelet Disord 2013;14:176. [Crossref] [PubMed]
- Franklin PD, Li W, Ayers DC. The Chitranjan Ranawat Award: functional outcome after total knee replacement varies with patient attributes. Clin Orthop Relat Res 2008;466:2597-604. [Crossref] [PubMed]
- Jo AR, Song EK, Lee KB, et al. A comparison of stability and clinical outcomes in single-radius versus multi-radius femoral design for total knee arthroplasty. J Arthroplasty 2014;29:2402-6. [Crossref] [PubMed]
- Schroer WC, Diesfeld PJ, Reedy ME, et al. Isokinetic strength testing of minimally invasive total knee arthroplasty recovery. J Arthroplasty 2010;25:274-9. [Crossref] [PubMed]
- D'Lima DD, Poole C, Chadha H, et al. Quadriceps moment arm and quadriceps forces after total knee arthroplasty. Clin Orthop Relat Res 2001.213-20. [Crossref] [PubMed]
- Stoddard JE, Deehan DJ, Bull AM, et al. The kinematics and stability of single-radius versus multi-radius femoral components related to mid-range instability after TKA. J Orthop Res 2013;31:53-8. [Crossref] [PubMed]
- Wang H, Simpson KJ, Ferrara MS, et al. Biomechanical differences exhibited during sit-to-stand between total knee arthroplasty designs of varying radii. J Arthroplasty 2006;21:1193-9. [Crossref] [PubMed]
- Kessler O, Dürselen L, Banks S, et al. Sagittal curvature of total knee replacements predicts in vivo kinematics. Clin Biomech (Bristol, Avon) 2007;22:52-8. [Crossref] [PubMed]
- Mahoney OM, McClung CD, dela Rosa MA, et al. The effect of total knee arthroplasty design on extensor mechanism function. J Arthroplasty 2002;17:416-21. [Crossref] [PubMed]
- Insall JN, Dorr LD, Scott RD, Scott WN. Rationale of the Knee Society clinical rating system. Clin Orthop Relat Res 1989.13-4. [PubMed]
- Gómez-Barrena E, Fernandez-García C, Fernandez-Bravo A, et al. Functional performance with a single-radius femoral design total knee arthroplasty. Clin Orthop Relat Res 2010;468:1214-20. [Crossref] [PubMed]
- Colwell CW Jr, Gelber JD, Pulido PA, et al. Early range of motion of the scorpio non-restrictive geometry cruciate-retaining total knee system. J Arthroplasty 2011;26:751-5. [Crossref] [PubMed]
- Hall J, Copp SN, Adelson WS, et al. Extensor mechanism function in single-radius vs multiradius femoral components for total knee arthroplasty. J Arthroplasty 2008;23:216-9. [Crossref] [PubMed]


