Incidence of postoperative delirium in patients undergoing total knee arthroplasty—an Asian perspective
Introduction
Total knee arthroplasty (TKA) is a widely performed procedure that has been successful in alleviating pain and restoring function, and its relevance has been increasing in ageing populations internationally (1). However, some patients experience suboptimal outcomes from surgery due to postoperative complications, one of which is delirium (2). Modern studies have evaluated the risk factors and incidence of postoperative delirium in post-TKA patients. A systematic review (3) investigating the incidence, risk factors, and prevention strategies for postoperative delirium analysed ten original articles, of which five original articles studied the incidence and risk factors of postoperative delirium in patients undergoing TJA—a total of three studies (4-6) done on its incidence as well as a total of two studies (5,6) done on its risk factors. The incidence ranged from 0% to 10%, whereas the independent predictors of postoperative delirium included age, history of psychiatric illness, decreased functional status, decreased verbal memory and the use of specific anaesthetic agents (benzodiazepines and opioids).
However, the epidemiology of these studies mainly focused on non-Asian populations. Our study seeks to investigate both the incidence and risk factors of postoperative delirium in patients undergoing TKA with a focus on the Asian population. This is especially relevant in today’s ageing Asian population (7).
Methods
Ethical considerations
The Institutional Review Board (IRB) of our institution approved the conduct of this study (CIRB 2017/2467).
Study design and participants
We conducted a retrospective review of 954 consecutive patients (1,016 knees) who underwent TKA by the senior author of this study in the year 2006. This particular year was chosen so that all patients had at least 10 years of follow-up following the TKA. All patients who underwent primary TKA were included in our review. Patients who underwent TKA at our tertiary healthcare institution were all part of a standard care pathway (Table 1) where they are assessed by the anaesthetists preoperatively, referred to the relevant specialists for optimization for surgery and are reviewed by physiotherapists before and after surgery. As part of our care pathway, patients are screened for alterations in their mental state in the postoperative period daily by simple questioning for orientation to time, person and place. Those who are found to be in an altered mental state are then referred to the psychiatrist for further assessment. Diagnosis of delirium was made by a psychiatrist based on the diagnostic and statistical manual of mental disorders (Table 2), 4th Edition (DSM-IV). The patients were separated into two groups: a non-delirium group and a delirium group.

Full table

Full table
Surgical procedure
Anaesthesia was either general or spinal. A midline skin incision was made and the joint was exposed through a medial parapatellar approach. The patella was then everted. A medial or lateral soft tissue release was then performed depending on the demands of the knee deformity. The menisci and the anterior cruciate ligament were excised. The posterior cruciate ligament was recessed but kept intact. The knee was flexed and the tibia was manoeuvred anteriorly for the bone cuts. Tibial bone cuts were performed with use of an extramedullary guidance jig. Thereafter, femoral bone cuts were performed with use of an intramedullary guidance jig. Flexion and extension gaps were checked and balanced with further soft tissue release. Trial implant components were inserted. Osteotomy was performed on the patella with the final thickness not less than 12 mm. The range of motion, stability, rotational balance, posterior cruciate ligament tension and patellar tracking were manually checked with the trial components in place. The definitive metal-backed fixed bearing implants (PFC CR; Depuy Orthopaedic International, Leeds, UK) were then cemented (Smartset; Depuy Orthopaedic International, Leeds, UK). All excess cement was removed and the surgical field irrigated copiously before wound closure in layers with sutures.
Outcome evaluation
All written and electronic medical records for patients were screened. Demographic information, perioperative details, drug usage, type of anaesthesia, perioperative complications, comorbidities, and pre-existing psychiatric conditions were derived from these records. Chronic drug usage was assumed if the patient had been on a particular drug for more than 3 months.
Statistical analysis
Incidence was calculated using standard formula. All statistical analysis was performed using SPSS v.18.0 (IBM Corp., Armonk, NY, USA).
Results
Incidence of postoperative delirium
The incidence of postoperative delirium was 0.59% (6/1,016). Half of those diagnosed with delirium (3/6) went on to have a documented history of dementia in the years following the index TKA.
Associations with postoperative delirium (Table 3)
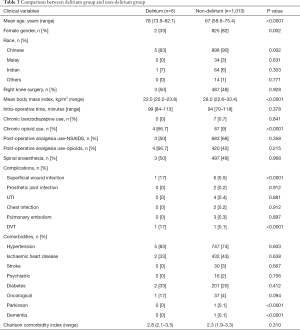
Full table
The median age in the delirium group of 78 years [interquartile range (IQR): 73.9–82.1 years] was significantly higher than that in the non-delirium group of 67 years (IQR: 58.6–75.4 years) (P<0.0001). The proportion of males in the delirium group of 67% was also significantly higher than that in the non-delirium group of 18% (P=0.002). It was noted that there was a significantly smaller proportion of Chinese in the delirium group of 83% versus the non-delirium group of 90% (P=0.002). Furthermore, there was a lower mean BMI in the delirium group of 22 kg/m2 than the non-delirium group of 28 kg/m2 (P<0.0001), and a higher proportion of chronic opioid use in the delirium group of 66.6% than the non-delirium group of 9% (P<0.0001).
A comparison of co-morbidities revealed a lower proportion of Parkinson’s disease in the delirium group of 0% than the non-delirium group of 0.1% (P<0.0001) and a lower proportion of pre-existing dementia in the delirium group of 0% than the non-delirium group of 0.1% (P<0.0001).
A comparison of postoperative complications also revealed a higher proportion of superficial wound infection in the delirium group of 17% than the non-delirium group of 0.5% (P<0.0001), and a higher proportion of DVT in the delirium group of 17% than the non-delirium group of 0.1% (P<0.0001).
Discussion
In the present study, the incidence of postoperative delirium following TKA was calculated to be 0.59%, which is very low at our institution. This is supported by Krenk et al., who reported the incidence to be 0% in a study size of 225 patients with a mean age of 70 years (9). However, the incidence varies across studies, which another study conducted by Jankowski et al., which reported the incidence to be 10% in a study size of 418 patients aged ≥65 years (5). A possible explanation could be that a standard care pathway is likely to be important in reducing the incidence of postoperative delirium (10). Another possible hypothesis is that a different diagnostic tool used to establish the diagnosis of delirium affects the calculated incidence. In both the present study and that of Krenk et al., the DSM-IV criteria was used, compared to the Confusion Assessment Method (CAM) used in the study conducted by Jankowski et al. This could potentially mean that the CAM is more sensitive and hence more useful in diagnosing delirium (3). Inouye et al. noted that the CAM has been shown to be sensitive, specific, reliable and easy to use for the identification of delirium (11).
We also noted some associations with postoperative delirium. Looking at the patient demographics, a higher mean age and male gender is associated with a higher risk of postoperative delirium whereas a higher BMI reduces the risk of postoperative delirium. A study done by Chung et al. shows that an increase in age by 1 year increased the risk of delirium by 1.15 times (12). Similarly, while the present study shows that men are at higher risk of developing postoperative delirium, there is no current literature to support this except a recently published a paper by Oh et al. which concluded that men are at higher risk of postoperative delirium after hip fracture surgery in a prospective cohort study (13). They attributed this to their underlying preoperative disease severity. Conversely, a higher BMI is associated with a lower risk of postoperative delirium, which we purport to be due to the nutritional status, though there has been no current literature to support this. However, Agar et al reported that a higher body mass index offered some benefit in survival in patients with delirium in palliative care (14).
Looking at the perioperative circumstances, chronic opioid use is associated with a higher risk of postoperative delirium. While there is no current literature to support this, opioid use postoperatively has been shown to not increase the risk of postoperative delirium by Nandi et al. (15). In the same study, they showed that benzodiazepine and isoflurane use perioperatively is an independent risk factor for postoperative delirium (15).
Looking at the postoperative complications, wound infection and DVT are associated with a higher risk of postoperative delirium. However we purport that this could be a confounding effect, as a result of the general health status of patients who had postoperative delirium being poorer as compared to those who did not.
Looking at the patient co-morbidities, the results suggest that Parkinson’s disease and dementia are associated with a lower risk of postoperative delirium. However, given that we only have such a small pool of patients diagnosed with delirium, and that only 0.1% (1/1,010) of the non-delirium group was diagnosed with Parkinson’s disease or dementia, the results are inconclusive. Chung et al. explains otherwise, that a history of dementia is an independent risk factor for postoperative delirium (12). Our study also noted that 50% (3/6) of patients diagnosed with delirium went on to have a history of dementia recorded, hence indicating a potentially stronger association between dementia and postoperative delirium.
Nonetheless, we do appreciate the limitations of our study. Firstly the method of identifying cases of delirium by retrospective medical record review is obviously prone to bias. However, we have confidence that the protocoled approach to the care of our post-TKA patients would have limited variability and inaccuracy. Secondly, given the small pool of patients diagnosed with postoperative delirium of 0.59% (6/1,016), there are limitations to the significance of our analysis. Thirdly, the gender biasedness towards females (81.4%) does affect the interpretation of our results. However, this is the demographic representation of patients undergoing TKA in our institution, which is difficult to modify. The strengths of our study include the use of prospective registry data making it valuable enough for trend analysis. We also had a relatively large cohort size and studied a variety of perioperative risk factors.
Conclusions
Incidence of postoperative delirium following TKA in our Asian population is low. This is likely contributed by use of a standard care pathway although prospective evaluation is necessary. Higher mean age, male gender, lower BMI and chronic opioid use may be associated with a higher risk of postoperative delirium.
Acknowledgements
We will like to acknowledge the staff at the Orthopaedic Diagnostic Centre, Singapore General Hospital for their assistance in retrieval of data.
Footnote
Conflicts of Interest: The authors have no conflicts of interest to declare.
Ethical Statement: The Institutional Review Board (IRB) of our institution approved the conduct of this study (CIRB 2017/2467).
References
- Talmo CT, Robbins CE, Bono JV. Total joint replacement in the elderly patient. Clin Geriatr Med 2010;26:517-29. [Crossref] [PubMed]
- Alfonso DT, Toussaint RJ, Alfonso BD, et al. Nonsurgical complications after total hip and knee arthroplasty. Am J Orthop (Belle Mead NJ) 2006;35:503-10. [PubMed]
- Bin Abd Razak HR, Yung WY. Postoperative Delirium in Patients Undergoing Total Joint Arthroplasty: A Systematic Review. J Arthroplasty 2015;30:1414-7. [Crossref] [PubMed]
- Postler A, Neidel J, Günther KP, et al. Incidence of early postoperative cognitive dysfunction and other adverse events in elderly patients undergoing elective total hip replacement (THR). Arch Gerontol Geriatr 2011;53:328-33. [Crossref] [PubMed]
- Jankowski CJ, Trenerry MR, Cook DJ, et al. Cognitive and functional predictors and sequelae of postoperative delirium in elderly patients undergoing elective joint arthroplasty. Anesth Analg 2011;112:1186-93. [Crossref] [PubMed]
- Rade MC, Yadeau JT, Ford C, et al. Postoperative delirium in elderly patients after elective hip or knee arthroplasty performed under regional anesthesia. HSS J 2011;7:151-6. [Crossref] [PubMed]
- Yoon H, Hendricks J. Asian Ageing: Contexts Of Change. Ageing Int 2003;28:115-134. [Crossref]
- Widiger TA, Frances AJ, Pincus HA, et al. Diagnostic and statistical manual of mental disorders: DSM-IV. 4th ed. Washington, DC: American Psychiatric Association, 2000.
- Krenk L, Rasmussen LS, Hansen TB, et al. Delirium after fast-track hip and knee arthroplasty. Br J Anaesth 2012;108:607-11. [Crossref] [PubMed]
- Radcliff KE, Orozco FR, Quinones D, et al. Preoperative risk stratification reduces the incidence of perioperative complications after total knee arthroplasty. J Arthroplasty 2012;27:77-80.e1-8.
- Inouye SK, van Dyck CH, Alessi CA, et al. Clarifying confusion: the confusion assessment method. A new method for detection of delirium. Ann Intern Med 1990;113:941-8. [Crossref] [PubMed]
- Chung KS, Lee JK, Park JS, et al. Risk factors of delirium in patients undergoing total knee arthroplasty. Arch Gerontol Geriatr 2015;60:443-7. [Crossref] [PubMed]
- Oh ES, Sieber FE, Leoutsakos JM, et al. Sex Differences in Hip Fracture Surgery: Preoperative Risk Factors for Delirium and Postoperative Outcomes. J Am Geriatr Soc 2016;64:1616-21. [Crossref] [PubMed]
- Agar MR, Quinn SJ, Crawford GB, et al. Predictors of Mortality for Delirium in Palliative Care. J Palliat Med 2016;19:1205-9. [Crossref] [PubMed]
- Nandi S, Harvey WF, Saillant J, et al. Pharmacologic risk factors for post-operative delirium in total joint arthroplasty patients: a case-control study. J Arthroplasty 2014;29:268-71. [Crossref] [PubMed]


