Favorable outcomes for female patients undergoing transcatheter aortic valve replacement?
Transcatheter aortic valve replacement (TAVR) is an established treatment for high surgical risk or inoperable patients with severe aortic stenosis (AS) (1-3). Interestingly, unlike percutaneous coronary intervention (PCI), approximately 50% of patients who undergo TAVR are female, despite the fact that female patients have fewer comorbidities than male patients (4-6). Furthermore, female patients have been found to have favorable outcomes as compared to male patients (5-10). However, to date, it remains unclear why male patients have a higher incidence of mortality after TAVR. Understanding this might help determine the effect of sex differences in patients with severe AS undergoing TAVR and should therefore be evaluated.
Chandrasekhar and colleagues assessed sex differences in patients who underwent TAVR using data from the Society of Thoracic Surgeons/American College of Cardiology Transcatheter Valve Therapy Registry (6). Between 2011 and 2014, 23,652 subjects (male: 11,844, female: 11,808) were enrolled in the study. To date, the study is the largest observational study investigating sex differences in patients treated by TAVR. Briefly, the main findings were as follows: (I) the female to male ratio of patients undergoing TAVR was in balance. However, there was an important sex difference with regards to age, prevalence of frailty, porcelaine aorta, presence of relevant mitral regurgitation, renal failure, and Society of Thoracic Surgeons (STS) score; (II) as compared to males, female subjects were more likely to undergo non-transfemoral TAVR. Moreover, TAVR in females was more often complicated by coronary obstruction, and females more often experienced conversion to cardiac surgery as compared to their male counterparts; (III) female subjects were observed to have a significantly higher adjusted risk of in-hospital vascular complications, resulting in a numerically higher rate of in-hospital bleeding events that did however not reach statistical significance; (IV) while no sex difference was documented with regards to in-hospital mortality or stroke, there was a significantly higher incidence of 1-year mortality in male as compared to female subjects.
The baseline characteristics of previous reports evaluating sex differences in TAVR are summarized in Table S1 (6-16). Consistent with the study by Chandrasekhar and colleagues, most of the previous reports showed that the prevalence of females was 40–60%, and that female patients were older and had a higher STS score than male patients. The overwhelming majority of patients undergoing TAVR in contemporary registries were treated for degenerative AS while bicuspid anatomy was rare. Hence, the risk factors for this population have some similarities to those for patients with coronary artery disease. However, in contrast to PCI populations, TAVR populations consistently feature a higher prevalence of females. The protective effects of estrogen might mitigate the progression of atherosclerosis in women (17,18). As a consequence, the proportion of males is higher among patients who undergo PCI. This discrepancy is still controversial. However, given the effect of estrogen, different risk profiles might help to explain these findings. Furthermore, female patients are older than male patients in the population which undergo TAVR. These findings might also be a reason to interpret favorable clinical outcomes in female patients. Whether there are factors for the insidious progression of AS remains to be elucidated. Thus, it is necessary to evaluate risk factors using multi-state models in a larger population to determine the influence of sex differences in patients undergoing TAVR.

Full table
According to several previous reports, there were significant differences between male and female patients in clinical outcomes after TAVR. These findings are described in Table S2 (6-16). On average, general anatomy is smaller in females than males, with a shorter coronary height and narrower femoral artery dimensions. Thus, the non-transfemoral approach is more likely to be used in female patients as a first-choice of access. Consequently, there is the significantly higher incidence of coronary obstruction, bleeding events, and vascular complications in female patients compared with male patients, as well as conversion to open surgery. However, since female patients also have smaller annuli, they tend to receive smaller valves and a narrower sheath compared with male patients. Female patients experienced more frequent vascular complications and bleeding events than male patients despite using a narrower sheath, which might be explained by their frailty. New generation devices that are miniaturized are mainly used as a first-line device for TAVR. These devices are associated with more favorable outcomes than conventional devices, as well as fewer complications and lower incidence of mortality (3). However, there are no reports in terms of the evaluation of clinical outcomes in sex differences after TAVR using new generation prostheses. Thus, it should be investigated to describe sex differences following TAVR in the real world.
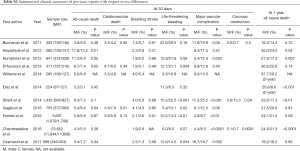
Full table
Notwithstanding the fact that there are some differences in baseline characteristics between female and male patients, the incidence of mortality after TAVR was similar for both sexes at 30 days. In contrast, the incidence of 1-year mortality was significantly lower in female patients than in male patients. However, Czarnecki and colleagues demonstrated that the 1-year mortality after TAVR was comparable between male and female patients when their baseline characteristics were matched by means of the inverse probability of treatment weighting (IPTW) (16). Only 999 patients were analyzed in their study, which is insufficient to evaluate sex differences in clinical outcomes after TAVR. However, given the results of the study, the findings of favorable outcomes following TAVR in female patients might be affected by the fact that females have fewer comorbidities. Furthermore, a meta-analysis performed in accordance with pooled analysis using a random-effect model to investigate 30-day and 1-year mortality after TAVR comparing male and female subjects has been published (19). In the study, the 30-day mortality was similar for both sexes, whereas the 1-year mortality was significantly lower for female patients than male patients. We do not have a proper understanding of sex differences in patients undergoing TAVR. Furthermore, the life expectancy evaluated by sex of patients treated by TAVR should be compared with that of the general population. This analysis might help to understand the real impact of sex differences in this treatment.
In summary, the largest observational study showed the assured findings with regards to sex differences in patients treated by TAVR. However, the study that matched baseline characteristics using IPTW has presented a different understanding of this issue.
Acknowledgements
None.
Footnote
Conflicts of Interest: The author has no conflicts of interest to declare.
References
- Leon MB, Smith CR, Mack M, et al. Transcatheter aortic-valve implantation for aortic stenosis in patients who cannot undergo surgery. N Engl J Med 2010;363:1597-607. [Crossref] [PubMed]
- Smith CR, Leon MB, Mack MJ, et al. Transcatheter versus surgical aortic-valve replacement in high-risk patients. N Engl J Med 2011;364:2187-98. [Crossref] [PubMed]
- Leon MB, Smith CR, Mack MJ, et al. Transcatheter or surgical aortic-valve replacement in intermediate-risk patients. N Engl J Med 2016;374:1609-20. [Crossref] [PubMed]
- Mack MJ, Brennan JM, Brindis R, et al. Outcomes following transcatheter aortic valve replacement in the United States. JAMA 2013;310:2069-77. [Crossref] [PubMed]
- O'Connor SA, Morice MC, Gilard M, et al. Revisiting sex equality with transcatheter aortic valve replacement outcomes: a collaborative, patient-Level meta-analysis of 11,310 patients. J Am Coll Cardiol 2015;66:221-8. [Crossref] [PubMed]
- Chandrasekhar J, Dangas G, Yu J, et al. Sex-based differences in outcomes with transcatheter aortic valve therapy: TVT registry from 2011 to 2014. J Am Coll Cardiol 2016;68:2733-44. [Crossref] [PubMed]
- Hayashida K, Morice MC, Chevalier B, et al. Sex-related differences in clinical presentation and outcome of transcatheter aortic valve implantation for severe aortic stenosis. J Am Coll Cardiol 2012;59:566-71. [Crossref] [PubMed]
- Humphries KH, Toggweiler S, Rodés-Cabau J, et al. Sex differences in mortality after transcatheter aortic valve replacement for severe aortic stenosis. J Am Coll Cardiol 2012;60:882-6. [Crossref] [PubMed]
- Erez A, Segev A, Medvedofsky D, et al. Factors affecting survival in men versus women following transcatheter aortic valve implantation. Am J Cardiol 2014;113:701-5. [Crossref] [PubMed]
- Sherif MA, Zahn R, Gerckens U, et al. Effect of gender differences on 1-year mortality after transcatheter aortic valve implantation for severe aortic stenosis: results from a multicenter real-world registry. Clin Res Cardiol 2014;103:613-20. [Crossref] [PubMed]
- Buchanan GL, Chieffo A, Montorfano M, et al. The role of sex on VARC outcomes following transcatheter aortic valve implantation with both Edwards SAPIEN and Medtronic CoreValve ReValving System(R) devices: the Milan registry. EuroIntervention 2011;7:556-63. [Crossref] [PubMed]
- D'Ascenzo F, Gonella A, Moretti C, et al. Gender differences in patients undergoing TAVI: a multicentre study. EuroIntervention 2013;9:367-72. [Crossref] [PubMed]
- Williams M, Kodali SK, Hahn RT, et al. Sex-related differences in outcomes after transcatheter or surgical aortic valve replacement in patients with severe aortic stenosis: Insights from the PARTNER Trial (Placement of Aortic Transcatheter Valve). J Am Coll Cardiol 2014;63:1522-8. [Crossref] [PubMed]
- Forrest JK, Adams DH, Popma JJ, et al. Transcatheter Aortic Valve Replacement in Women Versus Men (from the US CoreValve Trials). Am J Cardiol 2016;118:396-402. [Crossref] [PubMed]
- Gaglia MA Jr, Lipinski MJ, Torguson R, et al. Comparison in men versus women of co-morbidities, complications, and outcomes after transcatheter aortic valve implantation for severe aortic stenosis. Am J Cardiol 2016;118:1692-7. [Crossref] [PubMed]
- Czarnecki A, Qiu F, Koh M, et al. Clinical outcomes after trans-catheter aortic valve replacement in men and women in Ontario, Canada. Catheter Cardiovasc Interv 2017. [Epub ahead of print]. [Crossref] [PubMed]
- Stampfer MJ, Colditz GA, Willett WC, et al. Postmenopausal estrogen therapy and cardiovascular disease: Ten-year follow-up from the nurses' health study. N Engl J Med 1991;325:756-62. [Crossref] [PubMed]
- Grodstein F, Stampfer MJ, Manson JE, et al. Postmenopausal estrogen and progestin use and the risk of cardiovascular disease. N Engl J Med 1996;335:453-61. [Crossref] [PubMed]
- Conrotto F, D'Ascenzo F, Presbitero P, et al. Effect of gender after transcatheter aortic valve implantation: a meta-analysis. Ann Thorac Surg 2015;99:809-16. [Crossref] [PubMed]


