Survival of primary lung cancer patients in Brunei Darussalam, 1987–2012
Introduction
GLOBOCAN 2008 reported that, there were 1.6 million new cases of lung cancer (12.7% of total cancer cases) and nearly 1.38 million deaths (18.2% of total cancer deaths) worldwide (1). Four years later, GLOBOCAN 2012 reported that 1.8 million new cases of lung cancer were estimated in 2012, which accounted for 12.9% of the total cancer cases worldwide. It was also estimated 1.59 million deaths from lung cancer contributing to 19.4% of total cancer deaths in the same year. Lung cancer had been not only the most common cancer but also the most common cause of death from cancer worldwide. The overall ratio of mortality to incidence was 0.87, and considered a highly fatal cancer (2).
Didkowska et al. reported that lung cancer death worldwide was expected to increase to 2.9 million in 2035 (increase by 86% comparing to 2012). Though the scale of increase was different, the increase was expected in all regions. The increase was predicted to be highest in East Mediterranean region (by 123%) and Africa region (by 108%) (3).
Similarly in Brunei Darussalam, from 2004 to 2011, primary lung cancer was the most common cause of death among all cancers. It led to 16.5% and 19.5% of all cancer deaths in 2004 and 2011 respectively (4-6). Furthermore, the lung cancer mortality had increased from 9.1 per 100,000 population in 2009 to 12.7 in 2011 (6).
With this increasing burden of lung cancer worldwide, similarly in Brunei Darussalam, it is important to study survival of lung cancer patients as it reflected the effectiveness of the management of lung cancer (7). Though incidence and mortality was on the rise worldwide, survival of lung cancer patients had increased in several countries such as United States, United Kingdom (UK), Denmark, Australia, Canada and Singapore (8-11). One of the major factors which have great impact on the survival is the stage of cancer at the time of diagnosis (12). Unfortunately, most lung cancer patients were diagnosed at the advanced stage. For instance, more than 70% of patients were diagnosed in Stage III and Stage IV in the United States and Singapore (13,14).
To our knowledge, there was little information available on survival of lung cancer patients in Brunei Darussalam. Therefore, we aimed to investigate the survival of primary lung cancer patients from 1987 to 2012 in Brunei Darussalam, specifically, to determine survival rates and median survival times, the stages of cancer at the time of diagnosis, and differences of stages and survival between the first and second half of the study period to determine the trend.
Methods
Study design
This retrospective cohort study was conducted in 2013 & 2014, using 26-year recorded data from 1987 to 2012 in Brunei Darussalam.
Study population
We aimed for all primary lung cancer patients diagnosed in Brunei Darussalam as the reference population. As all cancer cases were recorded in the four district hospitals, and the Brunei Cancer Centre in Brunei Darussalam, all recorded cases were retrieved from the five institutions. Primary lung cancer cases diagnosed during the period from the beginning of 1987 to the end of 2012 were included without any exclusion criteria or sampling.
Data collection
A pretested data collection form was used to collect the data from medical record. Death information such as date and cause of death, were obtained from patients’ death record in the medical records and verified by death certificate obtained from the Immigration and National Registration Office of Brunei Darussalam.
Data collection form
We designed the data collection form, first by reviewing National Lung Cancer Clinical Audit form (15) and adding some additional information required for this study. Then, the form was pretested by collecting 20 cases without experiencing any significant difficulties. The form basically included demographic information of patients, smoking history, staging of cancer using the 6th TNM lung cancer staging (16), histology type and date of death or last seen.
Data analysis
Data entry and analyses were done using IBM SPSS version 20.0.0. (17). Descriptive statistics were used appropriately to describe numerical and categorical information of the study population. With regard to survival analyses, patients who died with primary lung cancer or complications of primary lung cancer were considered as events whereas those who were still alive at the last-seen date or died with caused of death other than primary lung cancer (e.g., car accident, heart attack) were considered as censored. The Kaplan-Meier method was used to analyse survival rates, survival duration and survival curve. Comparison of survival was done using log-rank tests.
Ethical considerations
This study was approved by the Medical and Health Research and Ethics Committee (MHREC) of Ministry of Health, Brunei Darussalam [Ref: MHREC/EDU/2011/10 (3), dated 16-Jun-2011]. The chief executive officer (CEO) of each hospital also gave permission to conduct the study. The Immigrations and National Registration office of Brunei Darussalam also gave permission to access patients’ date of and cause of death on their database.
Results
Demographic characteristics and smoking history
There were 630 primary lung cancer cases diagnosed during the period (1987 to 2012) and all were included. There were 137 cases diagnosed during the first 13 years (1989 to 1999) and 493 cases during the second 13 years (2000 to 2012).
Table 1 shows the distribution of demographic characteristics and smoking history. The mean age was 65 (SD 12.4) years old, ranging from 26 to 92 years. Majority was age between 51 and 80 (75.8%), male (60.4%), Bruneian (82.8%), residing in Brunei-Muara district (64.3%), Malay ethnic group (70.3%) and smokers (76.9%).
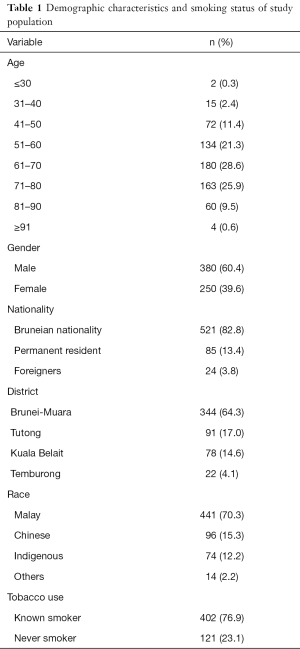
Full table
Stages of lung cancer & histology at time of diagnosis
The distribution of stages at diagnosis for 598 primary lung cancer cases is presented in Table 2. A total of 32 cases (5.1%) could not be included in the analysis as their stages were not stated in the records. From 1987 to 2012, majority of cases was diagnosed at Stage IV (42.5%), followed by Stage III (33.4%), Stage II (5.3%), and Stage I (9.2%). A significant higher proportion was diagnosed at late stage of cancer (Stage IV) in the second period (2000–2012) as compared to the first period (1987–1999) (43.4% versus 38.8% respectively, P=0.008).
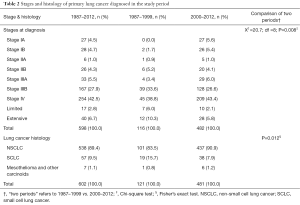
Full table
The distributions of type of histology are presented in Table 2. A significant higher proportion of non-small cell lung cancer was diagnosed in the second period as compared to the first period (90.9% versus 83.5% respectively, P=0.012).
Survival of lung cancer patients
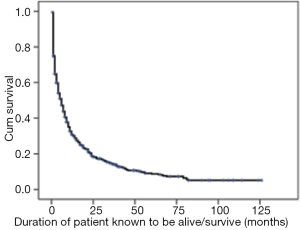
There were nine cases (1.4%) missing medical records after diagnosis and therefore, their survival durations could not be included in the analysis. The overall survival curve for 621 lung cancer patients (Figure 1) shows the rapid loss of survival after a few months of diagnosis. The median survival time was 6.1 months.
The survival rates and median survival time in month, and the comparison of these survival data between the two periods are presented in Table 3. Survival rates and median survival time of patients diagnosed in the second period had improved significantly (P=0.001) compared to the first period.

Full table
Specific median survival times for each stage of primary lung cancer for the whole study period, and also for each of two periods are reported in Table 4. In both overall and two periods, significant reduction of survival was observed as the cancer stage became more advanced. Specific survival curves for various stages for the study period are presented in Figure 2.

Full table

Discussion
There were only 137 cases (21.7%) diagnosed during the first 13 years but 493 cases (78.3%) in the second 13 years. Though there was no clear evidence for too low number of cases in the first period, we believe that this could be due to not seeking medical treatment in those days. This could be the same reason for the lower proportion of Stage IV during the first period than the second period. It might not be due to lack of diagnostic facilities as the medical facilities had been already equipped with CT scanners since 1986. Another reason could be poor hospital record system and missing records in those days especially after death of patients. What we obviously knew was that the hospital record system was improved and cancer registry was also established during the second period. Nevertheless, as we found in the literature worldwide (1-3), we believe that the incidence had increased to a certain extent throughout the study period.
Table 5 tabulates the comparison of distribution of stages between current and previous studies. Distribution of stages of both periods of current study was similar to other studies done in Singapore (14), US (9,13), UK (12), and Spain (18). This implies that early detection of lung cancer has been a big challenge even in the developed countries. This indicates that primary prevention of lung cancer is greatly important to reduce the burden of lung cancer. New method of early detection which is affordable, less invasive, easy to conduct (e.g., salivary biomarker) will be highly valuable.

Full table
Table 6 presents comparison of survival between countries from previous studies. For the period of 1987–1999, the 5-year survival of our study was poorer than other studies done in US (9), Denmark (20), UK (10) and Australia (10). However, for the period of 2000–2012, our result was comparable with Denmark (10) and UK (10) but poorer than Australia (10) and US (9). Similar pattern could be seen for 1 year-survival rate.
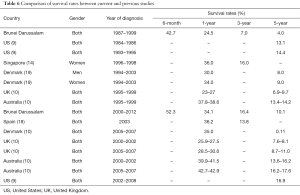
Full table
In this study, majority of primary lung cancer cases was diagnosed at between 51 and 80 years old, the youngest age was 26, two (0.3%) were below 30, and 17 (2.7%) were below 40. Though the mean age (65 years) at diagnosis in Brunei was comparable with the report for Singaporean women (65.3 years) (14), it was younger than the studies done in European countries, Australia and Canada where the mean age was 70.3 years (10). It is worth to investigate whether Bruneians were more susceptible for lung cancer at younger age.
The major weakness of the current study was possible missing cases especially in the first period (1987–1999) of study. However, the second period (2000–2012) data gave much reliable and valid information. It also had minimal and acceptable number of censored cases as lung cancer cases did not have long survival.
In overall, the survival of the current study was acceptable as it was comparable with some of the developed countries. However, survival still can be improved through early detection by adopting effective public health strategies such as by increasing public awareness of lung cancer, and guidelines for regular medical check-up for various risk groups. Finally effective anti-smoking campaign through public education will help to reduce overall burden of the disease.
Acknowledgements
Our most sincere thanks to the following department/organization: (I) Universiti Brunei Darussalam and Brunei Research Council for providing research grant for this study (S & T 22); (II) Ministry of Health and Medical and Health Research and Ethics Committee (MHREC) for giving permission to access the data, and ethics approval for this study respectively, and (III) the Immigration and National Registration Office of Brunei Darussalam to give access to death certificates.
Footnote
Conflicts of Interest: The authors have no conflicts of interest to declare.
Ethical Statement: This study was approved by the Medical and Health Research and Ethics Committee (MHREC) of Ministry of Health, Brunei Darussalam [Ref: MHREC/EDU/2011/10 (3), dated 16-Jun-2011]. The chief executive officer (CEO) of each hospital also gave permission to conduct the study. The Immigrations and National Registration office of Brunei Darussalam also gave permission to access patients’ date of and cause of death on their database.
References
- GLOBOCAN 2008 Presentation: Launch of GLOBOCAN 2008. International Agency for Research on Cancer 2010. Available online: https://www.iarc.fr/en/media-centre/iarcnews/2010/GLOBOCAN2008.pdf
- International Agency for Research on Cancer. GLOBOCAN 2012: Estimated Cancer Incidence, Mortality and Prevalence Worldwide in 2012. Cancer Fact Sheets (Lung). Available online: http://globocan.iarc.fr/Pages/fact_sheets_cancer.aspx
- Didkowska J, Wojciechowska U, Mańczuk M, et al. Lung cancer epidemiology: contemporary and future challenges worldwide. Ann Transl Med 2016;4:150. [Crossref] [PubMed]
- Ministry of Health BD. Health Information Booklet (HIB) 2004. Available online: http://www.moh.gov.bn/SiteCollectionDocuments/Health%20Indicator%20Booklet/healthindicators.pdf
- Ministry of Health BD. Health Information Booklet (HIB) 2008. Available online: http://www.moh.gov.bn/SiteCollectionDocuments/Health%20Indicator%20Booklet/HIB_2008.pdf
- Ministry of Health BD. Health Information Booklet (HIB) 2011. Available online: http://www.moh.gov.bn/SiteCollectionDocuments/Health%20Indicator%20Booklet/HIB_2011.pdf
- Coleman MP. Cancer survival: global surveillance will stimulate health policy and improve equity. Lancet 2014;383:564-73. [Crossref] [PubMed]
- Rachet B, Quinn MJ, Cooper N, et al. Survival from cancer of the lung in England and Wales up to 2001. Br J Cancer 2008;99 Suppl 1:S40-2. [Crossref] [PubMed]
- Howlader N, Noone AM, Krapcho M, et al. (eds). SEER Cancer Statistics Review, 1975-2009 (Vintage 2009 Populations), National Cancer Institute. Available online: http://seer.cancer.gov/csr/1975_2009_pops09/
- Coleman MP, Forman D, Bryant H, et al. Cancer survival in Australia, Canada, Denmark, Norway, Sweden, and the UK, 1995-2007 (the International Cancer Benchmarking Partnership): an analysis of population-based cancer registry data. Lancet 2011;377:127-38. [Crossref] [PubMed]
- Chia KS, Du WB, Sankaranarayanan R, et al. Population-based cancer survival in Singapore, 1968 to 1992: an overview. Int J Cancer 2001;93:142-7. [Crossref] [PubMed]
- Walters S, Maringe C, Coleman MP, et al. Lung cancer survival and stage at diagnosis in Australia, Canada, Denmark, Norway, Sweden and the UK: a population-based study, 2004-2007. Thorax 2013;68:551-64. [Crossref] [PubMed]
- Owonikoko TK, Ragin CC, Belani CP, et al. Lung cancer in elderly patients: an analysis of the surveillance, epidemiology, and end results database. J Clin Oncol 2007;25:5570-7. [Crossref] [PubMed]
- Tan YK, Wee TC, Koh WP, et al. Survival among Chinese women with lung cancer in Singapore: a comparison by stage, histology and smoking status. Lung Cancer 2003;40:237-46. [Crossref] [PubMed]
- Health & Social Care Information Centre. The National Clinical Lung Cancer Audit (LUCADA), Data Manual. Version 3.1.5. 2013. Available online: http://content.digital.nhs.uk/media/12788/LUCADA-Data-Manual-v315/pdf/LUCADA__Data__Manual_v3.1.5.pdf
- Sobin L, Wittekind C. TNM Classification of Malignant Tumors. 6th ed. New York: John Wiley & Sons, 2002.
- IBM SPSS Statistics for Windows. Version 20.0. New York: IBM Corporation, 2011.
- de Cos JS, Miravet L, Abal J, et al. Lung cancer survival in Spain and prognostic factors: a prospective, multiregional study. Lung Cancer 2008;59:246-54. [Crossref] [PubMed]
- Dalton SO, Steding-Jessen M, Engholm G, et al. Social inequality and incidence of and survival from lung cancer in a population-based study in Denmark, 1994-2003. Eur J Cancer 2008;44:1989-95. [Crossref] [PubMed]
- Jemal A, Bray F, Center MM, et al. Global cancer statistics. CA Cancer J Clin 2011;61:69-90. [Crossref] [PubMed]


